Today we continue with our mini-series on fighting the long defeat.
After you read this, please consider donating to our residents to get them to the US for an amazing surgery conference where they have been asked to present their hard work. As of writing this post, we are 40% of the way to our goal! Visit our fundraising page to learn more!
——————————————————————————————————————-
My specialization in pediatric otolaryngology is truly the best fit for me. For the most part, we are able to make a child’s life better and allow them to reach their full potential. All pediatrics works this way. Often we are faced with dramatic airway disease (stenosis, malformation or foreign body aspiration) that allows us to step in saving them from death’s door. Very rarely have I faced a child slowly dying from a malignant tumor who’s only chance at life is surgical removal. Such was the case of this sweet 10-year-old girl I met by chance one day in the capital.
I’m not sure if I ever mentioned it in past blogs, but in December I had the opportunity to join an Otolaryngology mission to Addis with Healing the Children. There, I was able to work with some really inspirational people. Watching fellow pediatric otolaryngologists triage, diagnose and treat Ethiopians was moving. They had been doing work in Ethiopia long before me, but I couldn’t help but feel a sense of pride for the work they were doing now.
I even had the unique opportunity to meet an Ethiopian pediatric anesthesiology fellow who was also part of the mission. I felt like for the first time I was able to explain my passion for the work here and have someone who understood the juxtaposition of American and Ethiopian life. It was enlightening and was my first real connection back home. A twinge of that deep gastric twisting occurred which is my body’s manifestation of homesickness.
One of the children that presented to that mission was trached 5 months prior after suffering from respiratory distress one week after a traditional uvulectomy (yes, this is done all over Ethiopia in children of all ages). He caught my attention as I walked through the waiting room due to his loud inspiratory stridor. Despite his trach, he still moved air through his larynx that was accompanied by this particular type of high-pitched stridor that I have come to associate with upper airway obstruction. A lateral Xray of his neck prior to the trach and a flexible scope of the larynx was highly suggestive a something bizarre in his subglottis.
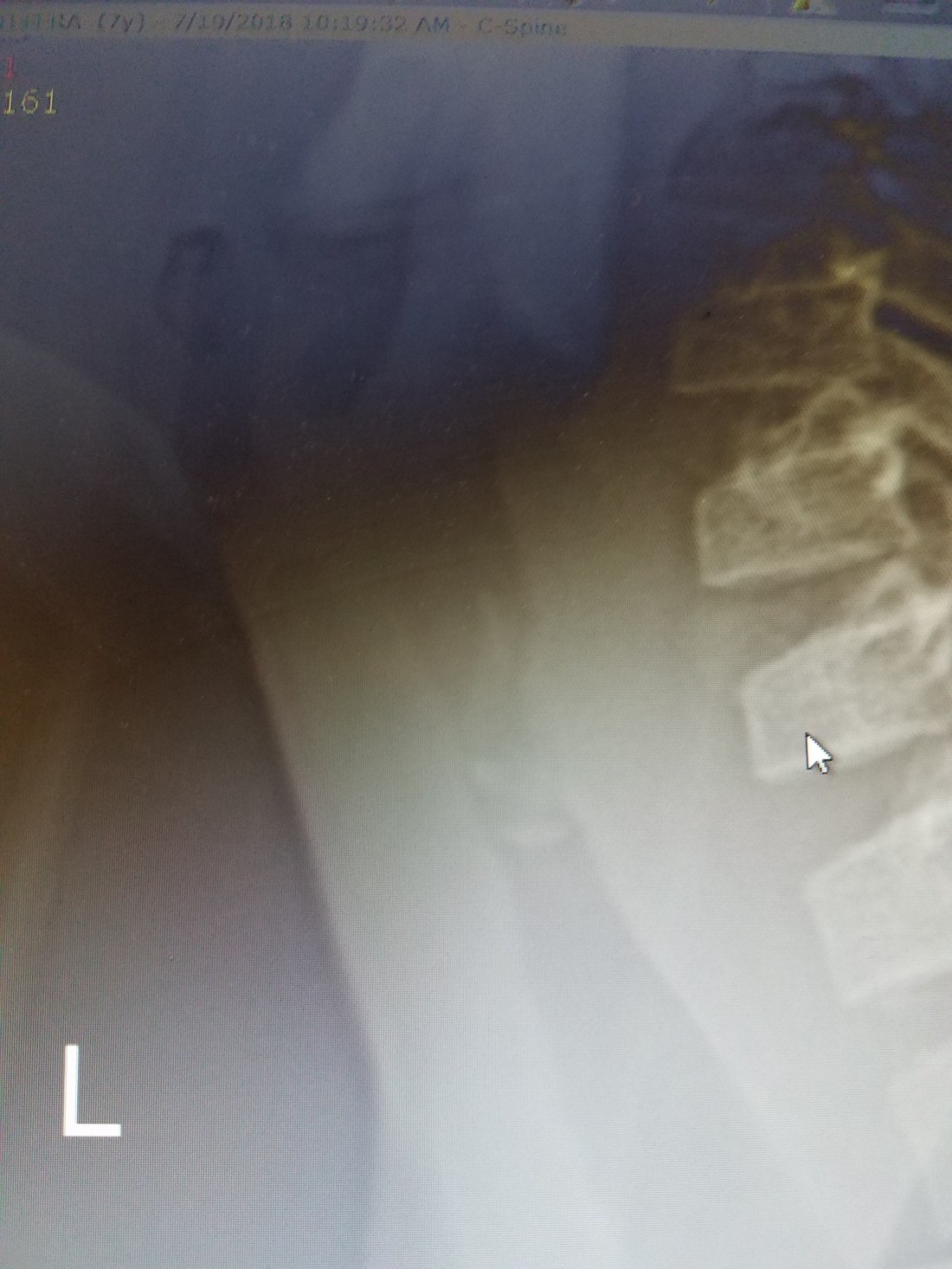
Armed with a spectacular team of pediatric anesthesiologists, a pediatric otolaryngology fellow and a seasoned pediatric otolaryngologists I was honored to lead this child’s bronchoscopy using the skilled hands of our otolaryngology fellow. After carefully planning our attack, the bronchoscopy revealed a chronic foreign body which we removed and spent the next hour cleaning out granulation tissue.

About a month later, I return to Addis and perform his follow up bronch at Black Lion Hospital. Housing one of the 3 otolaryngology training programs in the country. He had healed perfectly and we decanulated him the next day. The video of him, sent by the black lion residents is music to my ears.
Now, I mention this not only because its an excellent story of success, but also because while I was taking a tour of Black Lion with one of the senior residents, he said, “hey can you consult on this one patient we have?” When the patient was brought up to where we were, I first noticed the father in a squatting position with the expression of hopelessness painted over his face. Next to him was a small child wrapped in a headscarf. The “scarf sign” is a powerful one in Ethiopia. It almost always indicated that what’s underneath is unacceptable to society. This was a positive scarf sign.
This unfortunate 10 year old girl has suffered more than a year of painful facial swelling and deformation resulting in a cartoon-like malformation. Biopsies performed by the Black Lion team revealed Chondrosarcoma. A malignancy of the cells that create bone, this particular pathology is notoriously resistant to chemo or radiation. I didn’t need a CT scan to reconstruct what this lesion was doing to her head, but I sat in awe as we slowly scrolled through the images. This slow-growing tumor has pushed important structures laterally and superiorly (orbit and skullbase) and obliterated all non-vital structures through pressure necrosis (all structures of the nasal cavity, medial orbital wall, maxilla). Its pushing pathology rather than an invasive behavior adds to the suggestion of a low grade disease. Meaning, although the cells are technically malignant, their biologic manipulation has left them less aggressive than they have the potential to be.
Without metastasis, this child’s death would come in any of 3 agonizing forms: 1. Starvation from dysphagia, 2. Asphyxia from airway obstruction or 3. brainstem herniation from increasing intracranial pressure. Although it seemed crazy to me, her only chance at survival would be to remove this tumor which would result is a life-altering surgical deformity. With the family on board, we made arrangements to have them come up to Mekelle 2 weeks later to join the mission with Terry Day. I was going to tackle this with or without him, but his expert hands and decades of experience would give this child her best shot at life.
When they arrived in Mekelle, we had in-depth conversations with the father. Although somehow the right eye was functional, we may have to sacrifice it if the tumor got too close. The skull base’s integrity was unknown and a large CSF leak was entirely possible. And, whatever reconstruction that we could do after the tumor was removed would be temporary and much of it may die as she waits for adjuvant therapy. The ultimate goal would be a more definitive reconstruction 3-6 months later. It had grown considerably in the two weeks since I had seen here before and as we prepped for anesthesia and intubation I asked myself that same question I have so many times since coming here. Am I about to make this patient’s life better or worse?
As a young surgeon, I need to be careful with my decisions. 6 years of 80+ hours a week of surgical training does prepare you well. I can do a lot. However, I always force myself to check before I pull the trigger; should I do a lot?
She has suffered the past 2 or so years with a disfiguring, foul-smelling mass on her face. Although her father has probably grown to recognize this deformity as his precious daughter’s normal face (which I will find out to be the truth post operatively), not only is it not viable with life, she’s cast from normal society. Unable to experience what a 10-year old should. Clearing and maybe even curing her disease with surgery would certainly leave her disfigured. But worse than before? I don’t think so. The smell of necrotic tumor would also be gone, allowing her to approach within 10 feet of someone without the emotion of disgust directed towards her. This is a big, risky procedure, but worth it in all of our minds.
The surgery itself was an orchestra of sorts. Terry and I started on opposite sides of the tumor working with efficient speed to get down to disease and to isolate the normal structures of the face. Within an hour, we had the entire face degloved and the tumor isolated. A couple of osteotomies to release from the facial skeleton and the entire mass released with simple blunt dissection from the skull base.
It was something I’ve never experienced before. A massive well-encapsulated facial mass essentially detached itself from its compressed home. After its removal, I could imagine the epicenter of cancer replicating unchecked in the center of the bony midface. As it expanded from the center, normal bone was pushed, some necrosed, some further encapsulated the mass. From the massive defect left behind, you could piece together its origin. The right maxilla, partially eroded, was pushed anterio-laterally. The right orbital floor and medial wall were gone. There was no evidence of any other normal nasal structures apart from the choana and the hard palate was reduced to a thin shell covering the inferior portion of the tumor. The alveolar ridge of maxillary dentition was pushed into oblivion apart from two teeth on each side (which we would later use to anchor an oral obturator).
When it was out and the room irrigated, the aftermath was shocking. Seeing how cleanly this shelled out, we may have just cured her cancer, but it was just the beginning of her introduction back into society. Without knowing what the final pathology would be, we decided to close as much of the face as we could and pack the nasal cavity. We first used a titanium mesh to recon the orbital floor and medial wall and reattached the right medial canthus to the only rigid structure at midline, the frontal skull base. The right maxilla was in-fractured and secured to the contralateral maxillary alveolus with a titanium recon plate. This gave her a little anterior-posterior projection to her reconstruction. The cavity was packed off and the oral roof reconstructed with her left over hard palate mucosa to seal the oral cavity from the nasal.
To try to close the defect, we undermined the skin and fat from the right facial musculature and created an advancement flap. When it was all said and done, her face was closed, but it was free floating on nasal packing. The before and after was striking. She was certainly still disfigured, but her orbit was intact and on a brief glance, the deformity could go unnoticed.
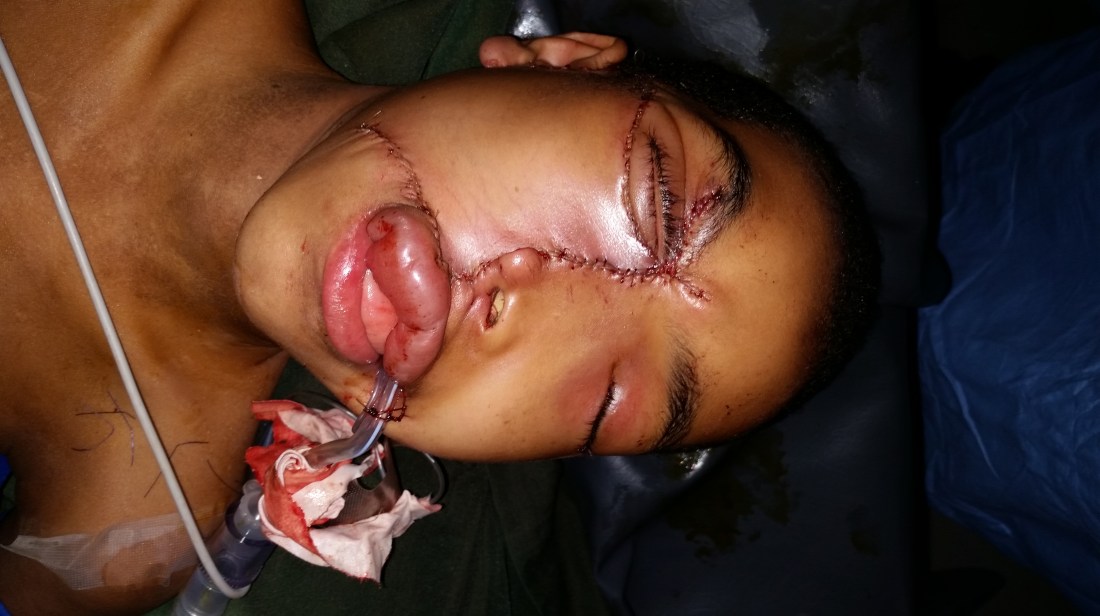
As the team was closing, I was called out emergently for a neonatal airway in the NICU. To get there form the OR, I have to pass through the family waiting area. While jogging to the NICU, I run into the father. He looked at me with deep concern, but knowing I had no time to explain, I just said “everything is good” in my broken Amharic. He burst with emotion, grabbing me tightly, kissing my hands exclaiming “thanks to god” over and over. I was right there with him, I felt his excitement and relief. I had been anxious about this procedure ever since I met her and I was thrilled with how well it went. I smiled and pried myself from his grasp and as I turned to resume my jog to the NICU, I saw all the families in the room sharing the same smile of hope this father had. Everyone in that tiny, overcrowded room had similar overwhelming anxiety and sick family members. A brief vision of success perhaps was projected to their own possibility of success.
By the time I returned from the NICU (a newborn with anoxic brain injury for unknown reasons and severe retrognathia couldn’t ventilate and needed intubation), our patent was extubated and being transported to the post operative unity to reunite with the dad. As is my routine, I sat down to drink a delicious whole milk/buna combination and write my post operative note. Afterward, I was excited to see the father’s excitement directed towards his daughter, but when I walked in, he was in a trance of disappointment and anger. I grabbed Yilkal to help me understand what was going in, but the father couldn’t articulate his displeasure. Just repeated “Eshi” (Amharic for “OK”) over and over and gestured for us to leave.
This job and the work I do here isn’t about my emotions, but I was really hurt by this reaction. We just brought his daughter back from certain death and he was angry at the job we did. I gave everything I had and utilized the entire day of an amazing head and neck team to achieve this and we are told to go away.
For me these big, dangerous procedures are still emotionally and physically draining. I didn’t have the emotional energy to debate my feelings about this so I internalized it for the time being. But I couldn’t help but check myself again, was this the wrong choice? I confidently answered, “no, we did the right thing.”
That night we debated the possibilities for his anger and decided it was most likely a combination of unacceptable expectations of facial appearance and the fact that he identifies his daughter as this wonderful young girl with a massive facial mass. Seeing her without it was like seeing a stranger. What we returned to him wasn’t his daughter in his eyes.
What we will all go through together over the next 6-12 months will be difficult. She may still need radiotherapy, she will certainly need multiple reconstructions and possibly be our first free flap as an institution. This is just the beginning of our relationship together.
—————————————————————————————————————
Next week we will conclude our mini-series with Hana from Bahir Dar.
Thank you for following along and please remember to to take a look at our fundraising page for our residents. We need your help!














