My first week in Ayder Referral Hospital in Mekelle, Ethiopia has been an extraordinary leap. Well, more like a free fall. Before I get into what the 1st week has produced, let me provide some background on the current environment. I’ll warn you now, some of the images in this post still shock me to look at. Continue while seated please. Also, for the non-medical reader, this may become a little dry and technical.
Our Department:
Although I don’t know much about the hospital yet, I do know that Ayder Hospital is the last line for complicated disease. People are referred from all over and some take 3+ days to travel to the hospital to see a doctor. Although most specialties require a referral from another physician, ENT also allows walk-ins. This unique group present to the front desk where they give their chief complaint. If it sounds like ear nose and/or throat related, they will be sent to the Outpatient Department (OPD) which is connected to the hospital. Up until this point, this was a narrow disease burden that really only pertained specifically to issues of the ear, nose and throat. Unlike in the states, where ENT departments in tertiary centers are Head and Neck surgeons doing everything from the clavicles to skullbase, ENT in Mekelle has been limited. For the most part, for example, airway (foreign bodies, stenosis and the like) go to cardiothoracic surgery, parotids/thyroids go to general surgery and most head and neck cancer (and cleft lip/palate) go to OMFS. The plan is for this to change.
The current staff is made up of Dr. Yilkal (most senior and head of the department). From my other posts, you know Yilkal and that is his “first name.” In Ethiopia, you are given a name, then you list your father’s name and then your grandfather’s name. Thus, everyone here goes by their given name or “first name.” And everyone calls me professor Josh. He is an extremely hard working guy who cares deeply about teaching. In the first years of the medical school in Mekelle, he even was asked to teach pathology to the pre-clinical medical students, some of whom have actually become pathologists. After Yilkal finished med school, he went to ENT residency in Egypt, where according to him, training was truly limited. He returned to Ethiopia and practiced for years before leaving to Senegal for a Head and Neck fellowship. Thus, he is the department’s “head and neck” surgeon. There are two other newer ENT’s Dr. Betelhem (Betty) and Dr. Medhanie (residency in Addis, the capital of Ethiopia) that I’ve really only met briefly and don’t know much about. They are both very nice and eager to learn. The 3 of them make up the ENT department.
In addition, last year Dr. Yilkal started a residency program which now has 4 R2s and 4R1s. 4 more fresh R1s are supposed to start in a couple months for a total of 12 residents. Clearly, this is far too many residents for the clinical exposure they have currently. Thus, most of them spend their time in clinic and only “operate” 1 day a week. In the clinic, even the R1s are in charge of examining and treating the patient. Only if they are concerned do they consult the “senior” AKA the attending. Nevertheless, every resident I’ve met is so thirsty to learn and grow and experience everything possible. Their eagerness and excitement far outshines that of American residents (no offense if any of you are reading this, I still love you). It has re-invigorated my desire to teach and reminded me why I belong in academics.
My First Patient:
On Monday, clinic started at 830am and I decided to join to watch. There are 3 clinic rooms and there are 2 residents in each room. A nurse assigns the long list of patients sitting in the overcrowded hallway to each of the residents and the day begins. Feeling awkward, out of place, and unclear where to stand/sit I started to set up my laptop to take notes of the clinic flow. It couldn’t have been 3 mins into the day when one of the R1s comes up to me and says “Professor Josh, can I please consult a patient with you.” Caught off guard, but honored, I sauntered into his room where a male (looked to be in his 40s or 50s) was sitting calmly in the clinic chair. He tells the patient something in Tigrinya and the patient begins to disrobe his neck scarf revealing the second worst neck mass I’ve ever seen in person (the prize-winning neck mass would surface just two days later; and then become an awake trach the day after that).
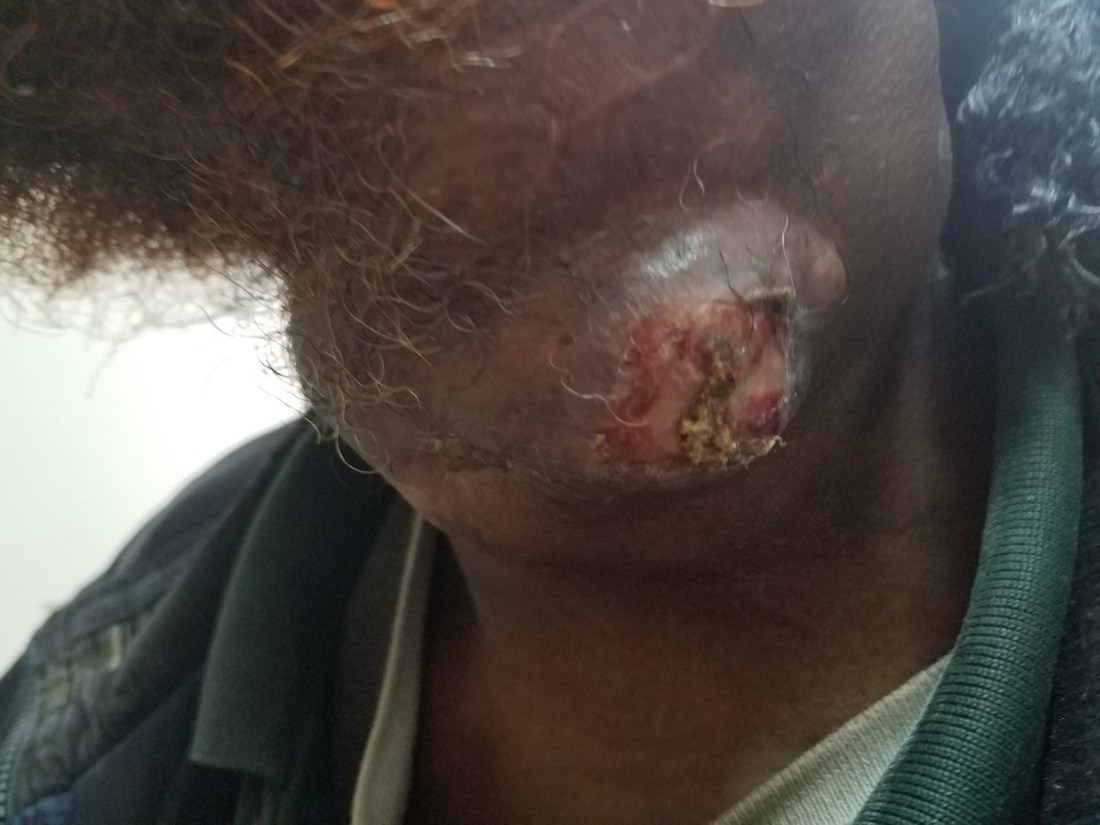
He struggles through his presentation to me (I made mental note to work on this) but I gathered that this mass has been growing steadily for 2 years following some type of incisional biopsy done at some other hospital. The patient had brought with him papers from two years ago with a path report indicated that his mass was suggestive of myoepithelial carcinoma.
I’ve seen a lot of head and neck cancer in my training, but I was stunned analyzing this presentation. If the path report was correct, in front of me was an extremely rare form of head and neck cancer presenting in a dramatic fashion. I had never seen this in training but knew from texts that at best 1/3rd are curable by surgery if the histology is favorable and there aren’t distant metastases. Chemo/rads is rarely helpful and adjuvant radiation is used with diffuse disease after surgically resected. The patient claimed he had no associated symptoms (dysphagia or increase work of breathing). The mass was rock hard, immobile and pushing the trachea toward the contralateral side. I felt no contralateral lymphadenopathy. He had no other physical exam findings, his lungs were clear and his cranial nerves were intact. The flexible scope of his larynx showed an effaced left piriform sinus, but an otherwise normal larynx with bilaterally mobile vocal cords. Still a bit shocked, we arranged for a CT neck and chest with contrast which he was able to obtain the same day. I was able to obtain the scans by going directly to the neurorads department where they burned a CD for me (I don’t have hot water in my house, but I can get a CT done on the same day…I’ll take it).
The CT shows the apparently classic very vascular multinodular appearance with areas of necrosis (or cyst formation). Other than some of the skin, vital structures appear to have mass-effect rather than invasion. The contrast-enhanced images are distinctly missing the left internal jugular vein (although it could just be compression), but intact arterial vessels. The common carotid is squished against the anterior scalene, but seems intact. There’s at least one ipsilateral big lymph node just under the mastoid tip (but honestly it could just be part of the multinodular mass). There doesn’t appear to be any contralateral positive lymph nodes which correlated with my physical exam. Internally I could hear the voice of one of my head and neck surgeons from residency chime in at this point, “Well, its certainly resectable.” Nevertheless, it would leave a large skin defect and an exposed carotid that would require muscle and skin to protect. Seems ideal for our workhorse, the Pec flap.
I’ll be reaching out to a number of my head and neck cancer surgeons back in the states to reach a consensus on treatment. Once that’s done, I’ll update the blog with the plan.
The Bleeding Baby:
Still a bit shell shocked from that experience a couple of hours later, one of the R2s called and asked if I could come to the NICU with him to see a baby that was “bleeding from the mouth.” He escorted me to the NICU which consists of a series of 3-4 partitioned rooms, separated by glass windows each holding around 10 babies. I distinctly noticed the lack of incubators and ventilators. The metal and plastic “cribs” were lined one next to the other. Our consultation was an 18 day old with persistent bleeding from the mouth since birth. He arrived to the hospital 5 days prior, cannot control the slow ooze and cannot seem to pass a feeding tube although bit nares are patent.
The baby looked tired and ill, his mouth rimmed with drying blood and chest speckled with coagulated blood. He was working hard to breathe without stridor, with occasional obstructions and apneic pauses. These would be followed by crying and bright red blood from the mouth. My exam of the oral cavity was normal and certainly noticed the blood coming from the oropharynx. The right lung barely moved air, sounding full of congealing fluid. I convinced the NICU team that this required an exam under general anesthesia but that I’d like to flex scope through the nose first. We grabbed the only flex scope available (a 4mm adult flexible laryngoscope). This showed, through waves of disorienting blood spatter, a mass ball-valving around the posterior cricoid area. This solidified my decision of the OR to see if anything could be done to make the airway safer. I knew intubation wasn’t a real option because there was no ventilator and tracheostomy would only be a temporary fix (there are very few baby trach tubes, besides no one could care for a trached baby here and they would need to spend the foreseeable future in the hospital). In my mind, I just hoped there was a simple fix that would buy this baby time to feed and grow.
I left the NICU to find the anesthesia team. Yilkal was involved by this point and lead me to the head of anesthesia. He was an extremely young-looking guy, but very nice and seemed very knowledgeable. As I explained the problem and how I wanted to handle the airway, I could see the terror and dread grip his face. Although they do pediatric surgery at Ayder, the concept of ENT handling the airway only after given halothane general anesthesia was unfathomable. I knew this was going to be a serious uphill battle and I was going to face it head on during my first week. Yilkal takes me to the storage room of the OR and opens a brand new Storz box full of unopened pediatric airway equipment. I was in heaven. Confident and ready to roll, one of the R2s come over to me with a new small strip of white paper. There, was written a K+ of 2.1.
Hypokalemia in an 18 day old in respiratory distress who was about to get general anesthesia with halothane made me pump the breaks. This type of analysis was beyond the reach of my training, but after speaking with the anesthesiology and NICU teams, we decided to hold off. The baby boy was no longer bleeding, the work of breathing improved and he was satting well with oxygen. The decision was to replenish the potassium to help avoid arrythmia on the table and to return to the OR the next day. I’ll probably question this decision over and over again in my career as he passed away that night.
We later learned from the mother that 4 of her other previous babies had died before 2 weeks of age due to bleeding from the mouth and respiratory distress. None of those had autopsies and she had no interest to obtain one now. I’ll never know if this was something we could have prevented, but I just wished we had had the opportunity to try.
The Teenager with Meningitis:
Presenting later that day was a 13 year old girl with severe meningitis with all the classic symptoms. Photophobia, neck stiffness, fevers and unable to move from the fetal position. She had apparently been this was for a number of days and had been placed on ceftriaxone and metronidazole for >72 hours. Despite this, she was worsening and the pediatric team ordered a non-con CT of the brain in hopes of identifying a source. No attempt to an LP was made. Following the CT, ENT was consulted to rule out Lemierre’s due the finding of a right thrombosed internal jugular vein (IJ). The finding was confirmed with an US. She never had odynophagia, neck swelling or neck tenderness.
She looked miserable, prescribed 1mg morphine three times a day, it was clear she haven’t felt relief in days and looked sicker than most others in the pediatric ICU. The only focal finding on exam was right postauricular tenderness (way out of proportion to hear headache; palpation made her flinch when otherwise she would sit motionless in the fetal position). No one had an otoscope, so we headed to radiology to review the CT. Normally, they would be uploaded to the PACS online system, but of course it wasn’t working.
In radiology, her CT revealed a chronically infected, sclerotic, coalescent mastoid with no apparent bony erosion medially or laterally. In the poorly windowed non-con CT, you can just make out the halo of the IJ through the neck on the right which was clearly different from the left. You see this in thrombosed veins as the vascular wall thickens and the inside fills with solid clot. You can diligently follow this finding up into the jugular bulb suggesting this is either neck disease propagating back into the sigmoid, or mastoid disease propagating into the IJ.
Finally armed with an otoscope, my suspicions were confirmed by a cholesteatoma retraction pocket in the superior posterior quadrant. We booked her for emergent surgery where a mastoidectomy confirmed a chronic cholesteatoma. When unroofing the sigmoid sinus, there was a sudden rush of pulsatile purulence under pressure. After skeletonizing most of the sigmoid and clearing the cholesteatoma into the antrum, the mastoid cavity was washed out, a finger of a glove placed as a drain and she recovered in less than 48 hours. Even though it was an easy diagnosis and relatively straight forward surgery, seeing her recover from death’s door to a normal happy teenager gives me feelings of elation that are utterly priceless. We will see her again in a month to book her for her definitive cholesteatoma surgery to help prevent this from happening again. Although evidence is not definitive on the treatment of the thrombosed jugular, because she is asymptomatic, I see no reason to treat it; it should re-cannulate over time. Nevertheless, the ICU here insists on treating with warfarin. Prolonged antibiotics will be given at discharge.
The next day, I proctored one of the attendings through a canal wall down for a large subperiosteal abscess from a chronic granuloma which she performed very well. That patient recovered well and was discharged for follow up in 2 weeks. I also watched how they performed an adenotonsillectomy which was relatively similar, but there is a lot of room to improve. At the end of that OR day, I was introduced to the worst neck mass I’ve ever seen.
My Worst Nightmare:
This 31 year old, otherwise previously healthy male presents with an enlarging neck mass over the past 2 months. Walking into the OPD, the odor greets me before I’m able to see the patients face. He has a head scarf, which I had learned from the patient the day before, is a bad sign. As he unwraps his neck, the odor intensifies and a brown saturated gauze falls from his neck revealing a horrific ulceration that pulsates with what I can only assume is his heart rate.
After the shock wears off, I remember the presentation was two months ago. Weary of that reality, we asked again when did you notice any swelling, he again said two months and also offered that he had been treating with a topical herbal medication which resulted in rapid growth and ulceration.
I knew this wasn’t squamous cell carcinoma and the diffuse nature of the mass along his entire right neck was suggestive of a highly proliferative disease. Similar contralateral lymphadenopathy further suggested lymphoma. Regardless of the diagnosis, it was advanced and progressive. We admitted him for wound care and an eventual open biopsy for definitive diagnosis. Theoretically, if we made a diagnosis and it was lymphoma, we could treat with chemotherapy. If the chemo miraculously worked then the ulcer would be small enough to treat with some type of flap. The problem in this plan revolves around oncology. Although there is a 7 story oncology center being built behind Ayder Hospital, there apparently is only one oncologist and he is a pediatric oncologist. There are internists that are interested in oncology, but not specifically trained in it. So the question becomes, if we can get a definitive diagnosis, will we have someone to treat with chemo? The alternative would be to ship down to Addis (the capital), but apparently similar problems exist there (plus they patient would rather pass here in Mekelle).
The patient also tells us he obtained an MRI 2 months ago and has the CD somewhere. We sent his family to find it. By this time it was Friday afternoon. Since no pathologists are here over the weekend and the specimen needs to be fresh, the decision was made to perform a bedside biopsy on the following Monday. Over the weekend, he will get much needed wound care and pain medication.
The Vascular Mass:
Also featured this week was a 14yo male (he actually looks 20) with a bizarre left submandibular and oropharyngeal vascular mass.
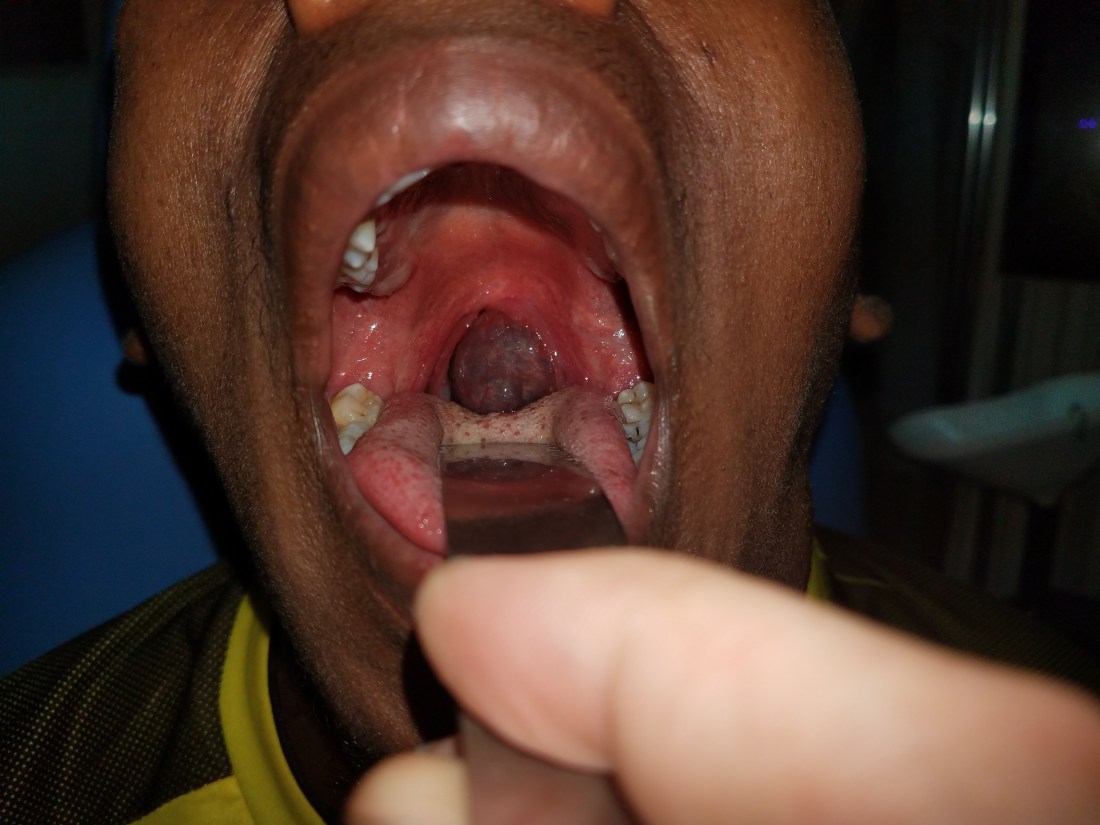
He had been followed by Yilkal in his private clinic for a couple of months and an FNA showed red blood cells (surprise, surprise). Other than the soft deformity of his left submandibular area and the dysphagia to solids, he had no symptoms. He was also sent for an MRI and CT which was also highly suggestive of a vascular mass. I haven’t had a chance to look up this scan yet, but once I do, I will add it to the blog.
I’ve had a couple of day delay in posting the blog because of a slew of emergent procedures including my first pediatric airway case! Teaser for the next post!


