Our 2nd part to our series on Neuronal tumors features a much more aggressive and destructive pathology: Plexiform Neurofibromas. This will be one of my most dense posts, but it is filled with interesting pictures and videos. So, grab a coffee and enjoy. Remember that the 3rd case here is the clinical perspective of my last post: The Other Side of Things which tells the story from the perspective of her father.
Neurofibroma’s aren’t new to me. Commonly presenting as an aspect of the autosomal dominant neurofibromatosis diseases, neurofibromas can grow on the nerve that controls balance and can grow large enough to cause permanent hearing injury. Thus, our specialty is often asked to join with neurosurgery to carefully remove these tumors as they encroach on the brainstem. Differing from Schwannomas (which we learned about recently), neurofibromas involve multiple types of abnormal nerve cells (not just Schwann cells).
Although I had read about plexiform neurofibromas in texts over the years of training, I’d never actually seen one until one of the surgeons in Ayder called me into the OR just 2 weeks into my stay here. There, she found a worm-like growth deep in the neck of a 1 year old child. It’s biopsy confirmed a plexiform neurofibroma.
I had no idea at the time, but this pathology was going to become one of the most difficult pathologies for me to treat over my year here. Plexiform neurofibromas are a rare sub-type of a benign nerve tumor that form into tangled nests of abnormal nerves, often described as a bag of worms. Historically, there is possibility of malignant transformation, but this is reportedly very rare.
Over my year in Ethiopia, we were introduced to 3 unfortunate children with extreme versions of this rare and bizarre pathology. We will walk through the treatment of these children together and explore the success and failures of each, in chronologic order.
18 year old with neck mass and respiratory distress:
Our first patient walked into our clinic in respiratory distress with a large right neck mass. He was an emaciated, shy and anxious teenager. He had trouble breathing but wasn’t dying. Our oral exam showed his right parapharyngeal area with a huge mass effect blocking nearly his entire oropharynx. Flexible scope from the nose showed the same of his hypopharynx. We couldn’t even find his larynx.

He openly admitted that he feels like he is going to die when he lies down, so CT scan wasn’t an option. Our ultrasound in clinic showed a massive heterogenous mass with a large area of fluid collection medially. The internal jugular vein and carotid were pushed laterally and posteriorly millimeters under the soft tissue of the neck. Using ultrasound guidance, we passed a spinal needle into the fluid collection and pulled 20cc of old blood. He didn’t feel much better. Thus, we did the safest thing possible, took him to the OR for an awake tracheostomy in order to buy us time to work this mass up.
Following this, we obtained a CT. Its location suggested a schwannoma, pushing the carotid sheath laterally, but this was like one I’ve never seen before. He informed us that he had seen a number of surgeons prior to his visit with us whom all told him his tumor was unresectable. I consulted countless of my mentors back in the states for advice. They suggest an MRI. Not much help (at the time, but in retrospect showed the real pathology, I had just missed it). The consensus was to proceed to surgery and remove the mass for definitive pathology and to help eventually decannulate him.
When he entered the OR, there was a power outage and I captured this ominous picture of him in the doorway of his own OR. Its one of my favorite pictures of the year.

The surgery itself was very difficult. As the video shows, the carotid had been pushed laterally and draped over the mass, sharing the same fascial plane. At the time, I had no idea if this was malignant or benign, but its smooth and thick capsule suggested benign. Nevertheless, we were careful to avoid injuring the tumor (to avoid spillage) and slowly freed the carotid from the mass.
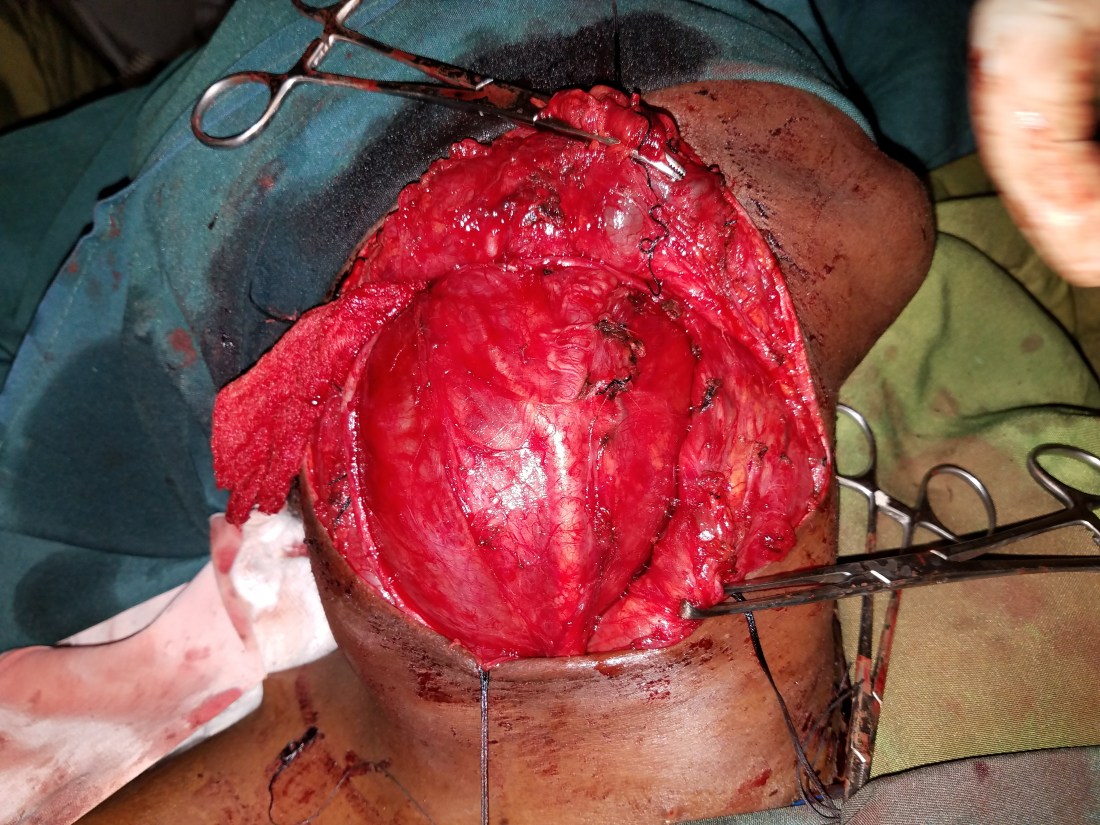
What was bizarre was that it looked and felt like a schwannoma, but its wasn’t attached to any nerves. Nothing superior, inferior or lateral. So, where did it come from? Once it was removed, we carefully inspected it for a break in the capsule. Nothing. We explored the neck for any sign of a primary tumor. Nothing. Admittedly confused, we washed the wound out and closed.
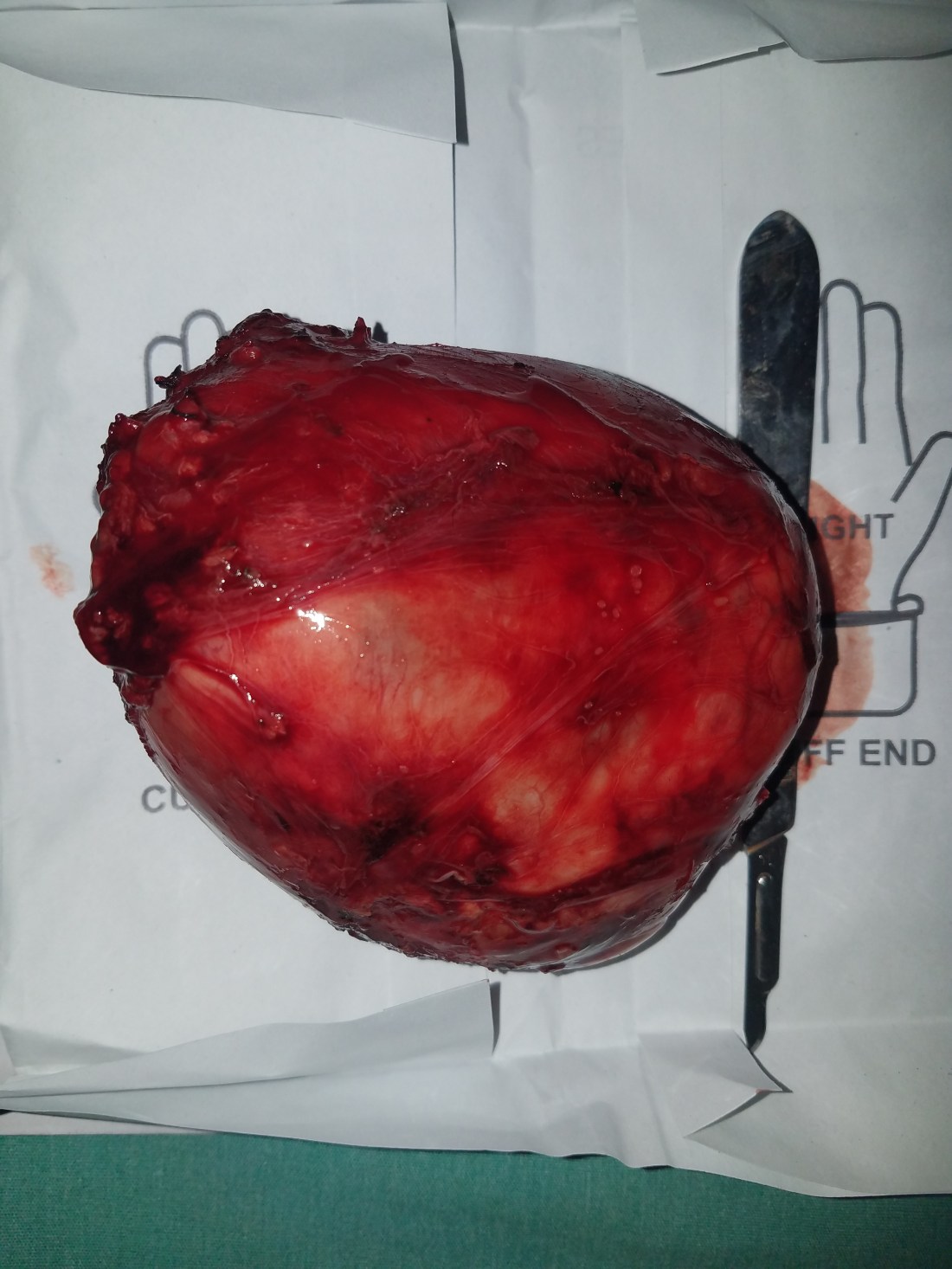
He recovered very well, but he did have a paralyzed vocal cord on flexible examination. This didn’t surprise me since there was dissection all over where the nerve was. Perhaps it was even paralyzed pre-op (this turns out to be the most likely answer). I did notice, however, that his right arytenoid tissue was abnormally swollen. But, being only 3 days from surgery, I convinced myself it would improve. We were able to decannulate him and his swallow was normal. He was discharged home.
He presented back to the clinic 2 weeks after surgery with his pathology report. Sarcoma.
What in the world!? How was there an isolated sarcoma (a malignancy from soft tissue) in the middle of his neck. This was very bizarre. I again consulted all my mentors and then some. Because the mass was completely encapsulated, we voted to watch and wait. On scope that day, the swelling was still there, mildly improved. Without any complaints, I asked him to return in one month. We will return to his story later.
1.5 year old with severe sleep-disordered breathing:
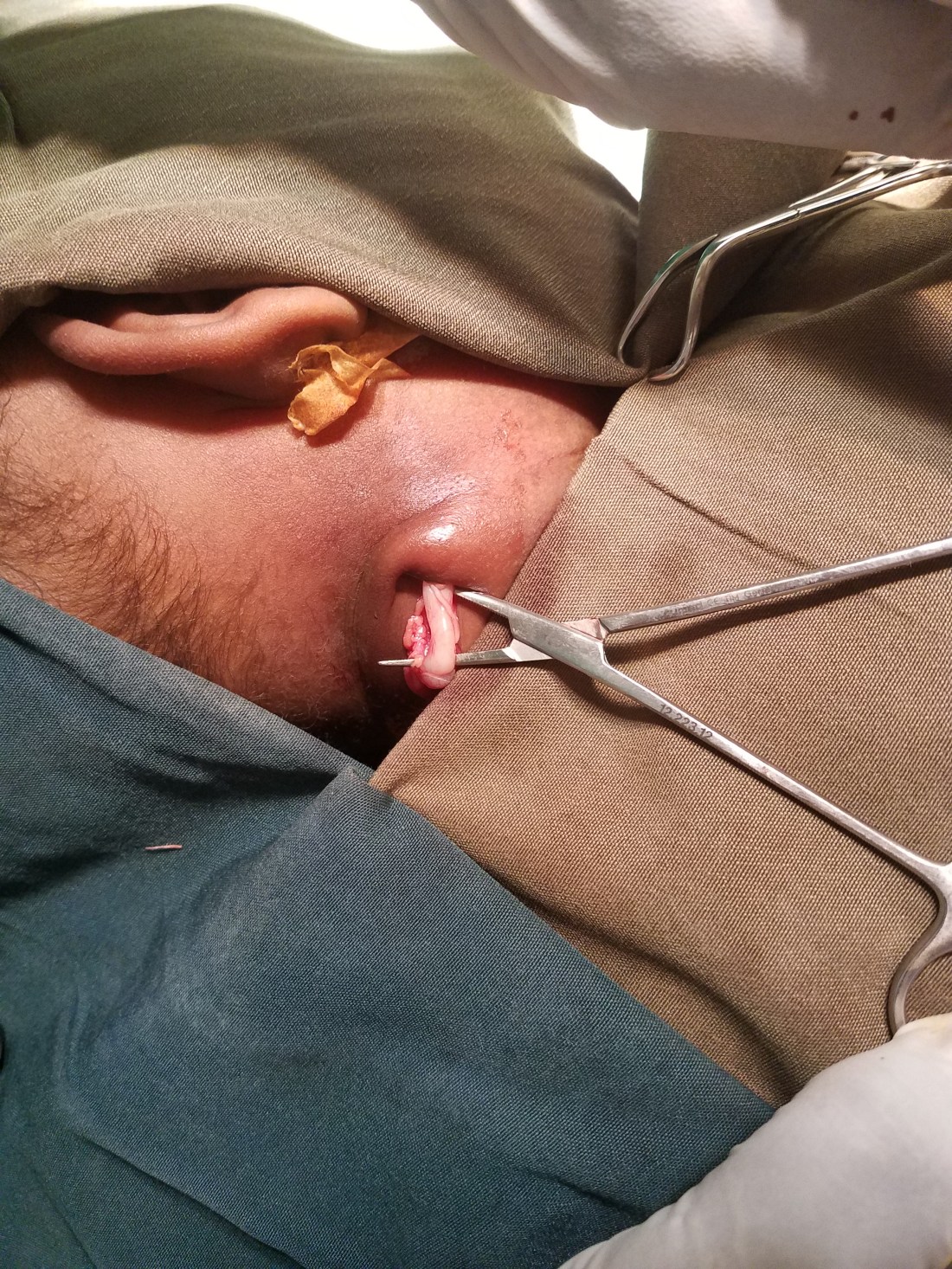
Enter our next patient. A 1.5 year old with severe respiratory distress while sleeping and mild while awake. He struggled to stay awake while on the back of his mother. I could clearly see his obstructive breathing while sitting straight up. His flexible exam was strangely familiar. In fact, It looked exactly the same as our 18 year old’s larynx. It was just a little more obvious that this one was immobile. Otherwise, the larynx was functional and open. I could appreciate how it would collapse during sleep, however. There was no palpable neck mass. Parents explained to us that he has been steadily getting worse over the past 6 months. I could tell that he was in no immediate danger, but he didn’t look good at all.
CT showed a hypoechoic mass in the arytenoid causing mass effect on the glottis airway. Duh. We took him to surgery expecting to find a chronic laryngocele, but after the first cut we found something much more interesting.
As you can see from the video after opening the larynx, we found a nest of neural-like structures. It looked exactly like the kid the other attending had called me into the OR evaluate weeks before. This looked like a plexiform neurofibroma. Because I knew so little about the disease and its real extent in this child, I decided to take a biopsy and get a rush on the results. I knew his obstructive breathing during sleep deprived his brain of oxygen needed to develop normally, but this obstruction wasn’t immediately life threatening. Placing a trach could be. That would be the standard of care back in the states, but here in Mekelle pediatric trachs come with a significant mortality risk.
We would maintain him on oxygen at night on the ward and he would recover just fine. While I encouraged the pathology department to rush this specimen to help dictate operative management, I started investigating laryngeal plexiform neurofibromas (and indeed pathology would later confirm this). They had been reported before in literature…with abysmal cure rates. Most would recur, some would die, all eventually required a trach or a laryngectomy. All reported literature I could find were case reports or case series, the least valuable form of publication, but at least it let me know that I wasn’t alone.
I talked to every pediatric and adult airway surgeon that would listen to me. None had seen this before. I found an “expert” in neurofibromas in Israel and reached out via e-mail. Amazingly he responded only to tell me there was no easy fix. Surgery is best, it will recur, this will be tough, good luck. There is a new medication that they are using to inject into these things, but its not something I’d be able to obtain in Ethiopia.
After a lot of thinking and planning, we decided to “optimize the airway” as best as possible. Essentially, remove as much as the tumor as possible, endoscopically, without compromising the airway or swallow. I didn’t want to make his life worse than it already was because I knew this would come back eventually. The weight of the tumor was causing collapse into the airway with each breath. It was worse during sleep because the muscular tone of the neck and pharynx were decreased allowing the negative pressure created by the diaphragms to suck in the heavy tissue to block the top of the trachea. Reducing the weight and redundant tissue may just prevent this collapse.
If we were to tackle something like this in the states, we would use powered instruments or, even better, a laser. We didn’t have any of this and our cold instruments were just too blunt to cut through this much tumor. So, we had to do something a little dangerous, use electrocautery endoscopically.
Now, we do this all the time in the states. Most tonsils and adenoids are taken out with electrocautery and it isn’t an issue. This is because we can titrate down the oxygen concentration that is going through the endotracheal tube to something close to atmospheric. Theres not enough oxygen in normal air to cause spontaneous combustion from the spark of an electrocautery. Unfortunately, the oxygen feeding the machines in the Mekelle ORs comes straight from the tank. 100% oxygen that isn’t mixed with air to dilute it. If theres even the tiniest leak around the tube then that much oxygen could easily ignite.
In training, we are hammered on what to do if this occurs. Its on every exam and is a favorite pimping question from attendings. Yank out the endotracheal tube (remove the fuel source; oxygen), pour water down the throat (extinguish the fire), and then re-intubate and clean out the lungs.
So, to make this safe, I asked the anesthesia team to turn off the oxygen so that the patient is just breathing room air. I remember how perplexed they were by this request. No surgery like this had ever been done in Mekelle, so I took the time to explain the rationale. Once the O2 was off, we got to work. Bucket of water at the ready.
The procedure was actually pretty easy and without complication. At the end, the lateral epiglottis was hanging in mid-air, so we performed a epiglottopexy suturing it to the lateral tongue base (forgive the Amharic music, we used this video for a presentation in the states).
His recovery was fantastic. He had a dramatic decrease in obstructive breathing and it didn’t take him long to be comfortable with feeding by mouth.
A couple days after performing this surgery, I had a sudden moment of realization. What if that first patient’s sarcoma was a malignant transformation of a plexiform neurofibroma and what I saw in his larynx was the same as this 1.5 year old child?!
I asked the residents to call that 18 year old back in. I wanted to ultrasound around his larynx and neck to search for a residual lesion. When he arrived to clinic, he was in great spirits. Compensating well with right sided vocal cord paralysis, eating, drinking and talking. Lucky for us, he compensated really well. We slapped on the ultrasound in clinic and what do you know, we found a bundle of crisscrossing hypoechoic lesions behind his right thyroid extending superiorly into the post cricoid area. I was sure he had a plexiform neurofibroma in there, but he was doing well and met no indications for surgical intervention. So we educated him and told him to come back and see us again in 3 months.
13 year old with massive neck and tongue lesion:
I saved the worst for last. This sweet, little girl scared the hell out of me. A fictional side of her story was the focus of my last post.
We were called to consult on a girl in the ER with a mass and respiratory distress. When we arrived, she had a positive scarf sign. This is the phenomenon I see far too often when a patient hides their horrifying head and neck mass from the public by wearing a scarf around their face. This sign has ridiculously high specificity.
I could hear labored obstructive breathing deep to the scarf and I could tell from her exposed eyes that she was scared. Not of me, which is common, but for what was happening to her. As we took off her scarf my heart sunk.
Her rigid and obstructive neck mass was dwarfed by her massive tongue lesion. As I watched her labor and I finish my physical exam, I noticed her mandible was malformed, widened with an open bite deformity. The only way she could breath comfortably was by protruding her tongue. I say tongue, but other than a shell of textures, it had been mostly replaced by this hard mass.
Her neck mass, mostly right sided not only severely deformed the trachea towards the left, but completely covered the front of it.
She couldn’t talk as the mass not only blocked air from escaping but also her lips from moving. She didn’t need to. Her eyes and cachectic body told me the entire story. This was the story of a child growing up in the poverty of rural Ethiopia with a small neck mass. One that grew slowly over the past 8 years. The pain of being socially ostracized slowly overshadowed by the sensation of strangulation as the back of her tongue limited the amount of air passing into her lungs. She would visit many traditional healers who would pray and burn her tongue and neck with hot irons with no avail. Faith was no match for this disease. Finally, as the iceberg was about to tip, she and her father made the 2-day journey into Mekelle to seek help. He knew she was dying, but maybe there was something out there for her.
From the topic of this post, we know what the diagnosis will ultimately be, but we had no idea at the time what this was. We just knew we had to do something.
With the airway completely compromised, intubation in the traditional sense was not an option. Our flexible scope of the nasopharynx showed that there was absolutely no path to the larynx. We couldn’t even find the larynx. I couldn’t explain how she was breathing as well as she was. I guess years of slow expansion taught her body how to compensate over time. Given the circumstances, the best and only option to protect her airway was an awake tracheostomy. Where, while awake, the airway is dissected out in the neck, opened and a plastic tube is placed.
I had never performed an awake trach on a child before. Ethiopia children are amazingly stoic and this girl I knew would be especially so. The problem was, the tumor pilled on top of the trachea for multiple centimeters. It would take a long time to dig through tumor to find the airway. Could she tolerate it the whole time?
I sat down with the anesthesia staff on duty, shared pictures and explained the circumstances. I could tell this was new territory for them, but their thinking was methodical and detailed. They were up for the task. We decided to partially sedate, place a plastic tube into the nose and help her spontaneously breathe with mask ventilation.
We explained to father how dangerous this procedure would be and that she might not wake up. He had clearly already come to terms with his daughter passing. He didn’t show emotion and told me that god will be with me in the OR.
We all agreed that anesthesia would be so light that if she ran into trouble, we would turn off the gas and she would wake up quickly. No matter what, we were going to optimize safety.
Even though it was a Saturday, there were a lot of people in the room. Everyone wanted to help. The anesthesia and ventilation through the nasal airway worked like a charm. With a heavy jaw thrust, she was able to fall asleep and remain oblivious to my digging in the neck.
An hour later, with a big chunk of the anterior tumor removed, we had an airway and we all could relax. She wasn’t going to die anytime soon. She had a chance now.
Under deeper anesthesia, I could fully assess the tumor. It became clear that the component in the neck wasn’t a lymphnode, but that is was all connected. One gigantic mass pushing up through the floor of mouth the replace the tongue. We found 40% of a normal tongue pushed off to the side, under the tumor.
Later, when the biopsy came back as a neurofibroma, we knew this was going to be near impossible to treat. Without radiation or chemo to help (they generally do not affect neurofibromas), surgery was her only, best option. Because we didn’t have microvascular equipment to create a free flap to reconstruct the floor of mouth, we decided to stage the surgeries. To truncate the tumor in half. Remove the intraoral part first, let it heal and then remove the neck. The final result would be a thin layer of tumor that would form the neo floor of mouth that she could easily live with for years. To hopefully be definitively treated once we could do free flaps.
The tumor was bulky and avascular. In the first surgery we were able to recon a functional tongue and in the second surgery, clear out 95% of the tumor. It seemed as if it originated from the hypoglossal nerve, perhaps.
It was around this time that our 18 year old followed up again, now suffering from obstructive breathing problems. We agreed to take him to the OR to endoscopically debulk him as well. This video shows the aftermath of that debulking.
He is about 3 months out now and doing very well without complaints. We will likely have to do this again, but only time will tell.
Back to our little girl:
She stayed with us for 3 months as we tried to rehab her swallow. We had to reverse 8 years of abnormal swallow without the expertise of speech therapists. It was very slow and she seemed completely disinterested in swallowing. Perfectly happy to have her feeding tube do the work.
But no matter what was happening to her that day, she always greeted me with the biggest, most genuine smile when I would see her on rounds. Its as if she was trying to hide the smile, but couldn’t smother her excitement. For 3 months, it was the happiest moment of my day.
She also caught the attention of visiting nurses, who would cherish the opportunity to take selfies, which she loved.
When she was finally discharged, she was eating and drinking (using the feeding tube to supplement) and in good spirits. Her trach remained in place with plans to decannulate down the road.
I knew, however, that perhaps we were discharging her in too good of a condition. Rural families have the tendency to not follow up if they feel things are going ok. Only to return when things are, again, terrible. She was discharged about 3 weeks ago as I write this and I’m worried I’ll never see her again. Already, her father and relatives refuse to answer our calls.
My only hope will be the sister of our most recent laryngectomy patient. The two of them shared a room and the sister basically became a second mother to the girl. Helping her eat, reading her books, even brining her new clothes. This is a unique aspect of medicine here that will be a topic of a future post. I hope that this sister can find this little girl so that we can continue to help her. But perhaps just as important, so that she can continue to be in my life.







