In just 1 year, I’ve seen 10x the number of nerve-related tumors than I have in my 11 years of medical training. Each has similar characteristics, but everyone is unique and full of learning points. I’ll group 5 different cases into two posts: Schwannomas and Plexiform Neurofibromas.
Today we will begin with the more light-hearted ones: Schwannomas.
Lets begin with the more recent patient. A very pleasant 73 year old lady presenting with her daughter. She first entered our clinic on a day I was in the OR. So, I was first introduced to her via a picture of her lesion sent by one of my residents (sorry its blurry, but you get the point). It was a raised ulcerative lesion of the face it appeared. They told me they did a biopsy and that she will return with the results. She was scheduled for my clinic when the biopsy result was due.

When she arrived, that same raised ulcerative lesion that she presented with was the last thing that attracted my eye. Due to the fact that her right eye was gone. Clearly surgically removed with a very clean and well-healed socket. And, on the same side, a massive neck mass creating asymmetry from a mile away.
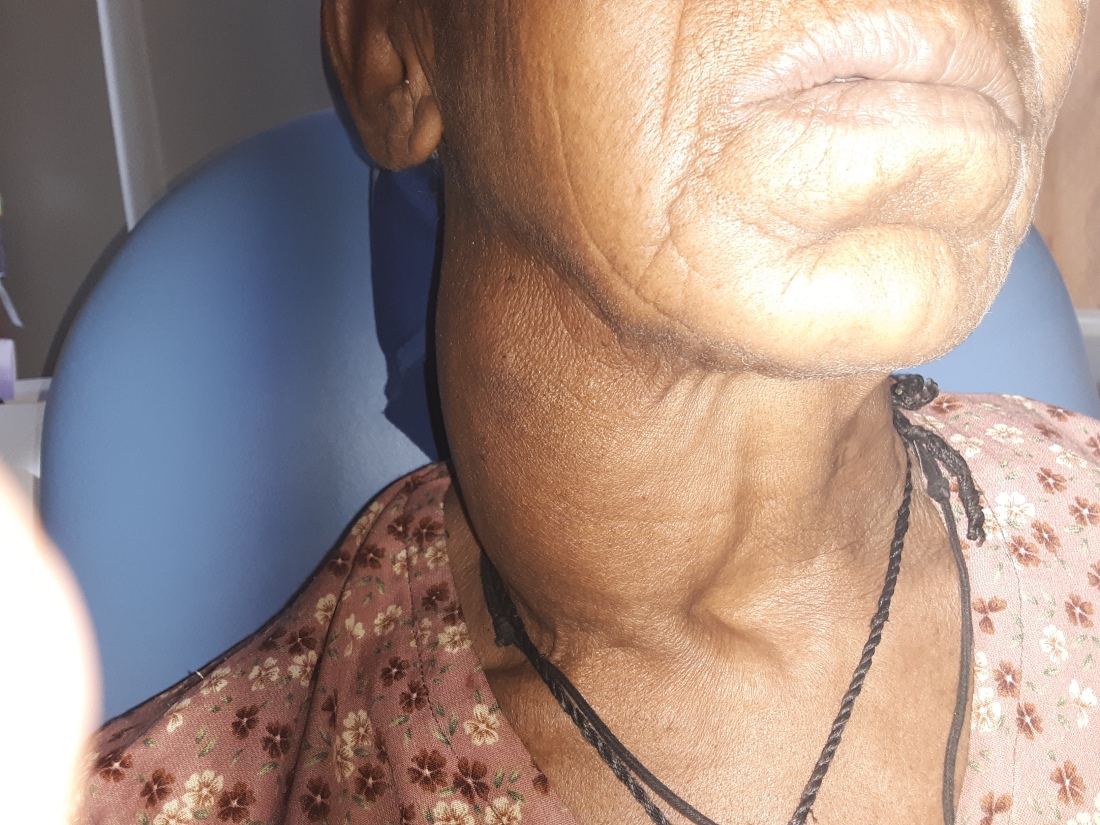
With the path report reading squamous cell carcinoma (SCC), I started to become worried for her. I put together this story of SCC involving the orbit that was removed some time ago, but now has not only recurred locally but has caused a massive metastasis in the neck. Really terrible prognosis keeping in mind that the waitlist for radiation is at least 1 year.
However, as I began to hear her story 4th hand. Mother to daughter, daughter to my resident, Tigrinya speaking resident to Amharic speaking resident, and then finally resident to me; it painted a different picture. The eye part was probably correct. There was an old mass affecting her eye which was removed 3 years prior by a mission team from America in a different hospital. She couldn’t remember what it was nor did she have any records (a common problem). BUT, the good news was that the neck mass had been there prior to the eye surgery, in fact, for decades, slowly growing. The prior surgical team were ophthalmologists and did not want to venture into the neck, my resident explains. And, if you’re super astute, you noticed another lesion on the tip of her nose. That had been there for her entire life and had not changed in size.
By now, all the residents are well trained in the management of head and neck cancer. I challenged him with this complicated case. “What do we do?” I asked. I couldn’t have been more proud of his response. He correctly identified the ulcerative mass as the bigger issue. With pathology returning SCC, we needed to assume it was recurrent and thus perhaps more aggressive than normal. Not to mention that we didn’t know the post-surgical anatomy with the eye now gone. Thus, imaging of the face. With XR, CT and MRI as the options, he correctly decided CT. The skin is thin here and we need to look into bony invasion which is best appreciated on CT.
“What about the neck mass?”. Well, he continued. If this does involve the bone of the face, its upstaged to a T3 which necessitates a neck dissection. If we have to go there anyways, why don’t we evaluate the neck mass?
“Sure,” I respond, my typical leading response that my residents hate, they know follow up questions are coming. “Is there any other way to evaluate the neck without opening it up?” His eyes light up when he realizes where I’m leading him.
Our residents LOVE using the ultrasound. As surgeons, we need immediate satisfaction and the ultrasound provides a look deep into soft tissues without any harm. All of the residents have become excellent at exploring the neck for answers using this simple, cheap technology.
He also explains we can look around for malignant appearing lymphadenopathy. “Yup,” I respond. “So go do it.” I find myself often giving my residents this sarcastic, laissez-faire attitude when they are working up a patient. Not to be rude, but to emphasize that they know what they are doing and should continue to practice accordingly. They are all reaching the point in residency where the knowledge acquired meets clinical intuition. It’s one of the most important times in medical training, but it’s hard to trust. To believe in yourself. My tone serves to let them know that I’m here for them, but they are 100% on the right track. I think they appreciate that…I hope…or they just think I’m an Asshole.
Anyways, as he readies the ultrasound and slaps on its iconic blue goo, he begins to define normal anatomy. Problem is, its not normal. Around this massive single hypo-echoic (less dense than muscle) neoplasm he identifies the common carotid artery being smashed medially against the thyroid and trachea. So much so that the trachea itself (made of semi-rigid cartilage), is bent, deviated and narrowed slightly. She didn’t seem to mind, though. Conversely, the internal jugular along with the sternocleidomastoid muscle are pushed so far laterally, they are almost in the back of the neck. This manipulation of tissue with its clinical course and appearance on ultrasound narrows the differential down dramatically. This is probably a Schwannoma. Probably one originating from the vagus nerve. A massive one.
Typically the carotid, internal jugular vein and the vagus nerve all hang out in wrap of connective tissue called the carotid sheath. The vagus nerve nestles itself between the pulsating behemoths, safely protected from injury from the outside world. This is actually one of my favorite places to dissect. It’s hard to explain, but the tissues feel nice when you bluntly dissect around one of the largest artery and veins in the body. If you’re confident, it’ll open up invitingly as if it can sense fear. Only the cautiously fearless can explore it’s contents.
I remember first seeing these vessels early on in training. My attending surgeon proficiently dissected around them with beautiful, elegant strokes. But, the knowledge of what would happen if one was injured paralyzed me with fear. If the common carotid were injured the patient could die in a minute from blood loss or cause brain damage from lack of oxygenated blood supply. An example of how medical knowledge does not match surgical intuition. It took years of seeing and touching this space to appreciate it. Only after you learn how to repair these injuries can you confidently dissect them. Part of being a proficient surgeon is being able to immediately fix issues that arise during surgery.
Since we saw these two vessels being pushed in opposite directions, one can make an assumption that it must be coming from the vagus nerve. Its the only thing that sits between them. Logic permits that train of thought for sure. And, given that she told us it had been there for years, its likely a benign process. Putting it all together points to schwannoma as the most likely culprit.
Every big nerve in the body have cells that wrap around it. They act as insulation of sorts to allow for faster and more accurate neural conduction. These are called Schwann cells. If they develop a mutation resulting in the uncontrolled division of cells, they form a schwannoma. Other than the compressing tissues, they generally don’t cause harm and most people have them without ever knowing. Seeing that she was 73 and seemingly unaffected by this mass, it could very well stay there for the rest of her life. We explained this to her. She gave me the typical response from our Ethiopian patients. “I want it out. If you can take it out, get it.”
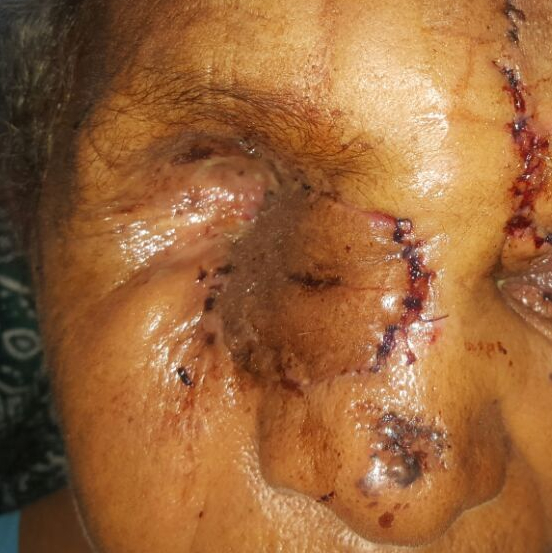
First, we shifted focus to the SCC. After reviewing the CT and seeing no bony invasion, we took her to the OR. Here we made a wide margin around the ulcer, removed all the soft tissue around it and even the bone beneath it (to be 100% sure there was no tumor left). This left a large soft-tissue defect and a very small bony one. This was easily reconstructed with a left paramedian forehead flap using skin from the forehead to cover the defect. It stays there for 3 weeks to develop its own blood supply before being truncated away from its artery and vein.
Surgeons out there would say “shit, that flap looks dusky.” I agree, but it had good blood flow. Promise. I can’t explain its color.
We then turned out attention to the neck, opening it up not because of the mass, but the statistical probability of there being metastasis to the lymphnodes. We performed a neck dissection to remove all of them in a certain area which uncovered the massive benign-appearing tumor.
A tiny bit of dissection revealed its true origin. We discovered the internal jugular vein lateralized, the carotid medialized and the vagus nerve sitting on top!
We were now encountering and even rarer diagnosis. A Schwannoma of the floor of the neck. Here it could be the sympathetic plexus (which send important neurological signals to the head and neck), the phrenic nerve (controls the diaphragm and breathing), or some random unnamed nerve. The morbidity from removing the sympathetic chain is minimal, but removing the phrenic nerve can cause some problems, especially in the elderly.
A little deep dissection showed us the phrenic nerve. So, out the mass came.
Any other head and neck surgeon could easily make the argument not to take out this mass. You’re almost certain it is benign, it has been there forever with minimal symptoms and you could make things worse for her. However, if we cure this cancer, she has a lot of life to live. It is possible this mass would start causing real compressive symptoms turning its removal into an urgent case. But, most importantly, we were already in the neck. The scar tissue that would form would make a future dissection riskier. Important structures would become sticky and immobile. Perhaps the phrenic or vagus couldn’t be identified and would be mistakenly removed with the mass (I’ve seen many case reports like this).
Whatever the patient’s decision comes to be, informed by the facts, tends to be the correct decision in these cases.
Weeks later, at her second surgery to release the pedicle, her face looks great, the margins are clear on pathology, the lymphnodes were clean of cancer and she has no appreciated morbidity. I say appreciated because taking the sympathetic chain out certainly does change physiology, but some people would never notice, especially someone without an eye on that side.
AND, the pathology on the neck mass came back as an ancient schwannoma. I had never heard of the ancient part and quickly looked to my pathology textbook for answers. All it means is that there was evidence of chronic long-term change in the tumor….boring. So, final pathology: 1. Recurrent T2 squamous cell carcinoma of the face with clear margins and no metastasis to the neck and 2. An old schwannoma of the sympathetic nerve. COOL!
———————————————————————————————————————-
Our similar case I’ll be much quicker with because of its similarity. This time the scene is Black Lion hospital in Addis and the patient is a 16 year old girl. Presenting with a massive slow-growing neck mass. Before I arrived, the team had obtained a CT which showed the same manipulation of anatomy as the case above.
The residents down in Addis do not get the same education our Mekelle residents do. Open neck surgery is basically non-existent for them. So this case and others we performed together over the year are exciting and rare. The eagerness of these learners brings so much joy and excitement into my life. This case, indeed, may be something they never see again in their career.
Again expecting a vagal schwannoma, once we dissect the tumor out, we run into the exact same anatomy. A sympathetic chain schwannoma. This time, the good and the bad are different. With the tumor in my fingertips, we debated the plan out loud, together as a group of scientists. Sacrificing this nerve would leave here with a visual deformity of her face (her upper eyelid would lag down farther than the left), the pupil of the eye would have trouble dilating and basic functions of her face would be altered (tearing, sweating, salivary production, heat control).
I posed the question to the group. The anesthesia team, focused more on the surgery the entire time, also leaned in to answer. Would her lid lag make it difficult for her to find a husband? Ethiopian culture, in most places, still gives economic value to being able to “marry off” daughters. Those unsuitable for marriage could be ostracized.
By this point there we probably 20 people in the room (including an American nurse that had joined me from Mekelle on a mission). Every single one said it wouldn’t matter. Ok, an easy decision there.
What about a lifetime of abnormal neural signaling? No consensus there. And I agree. For this matter, the risk of the mass getting large enough to cause serious issues in her lifetime was very high (seeing that it was already massive and she was only 16). So, out the tumor came.
What I’m ignoring here is that we assumed this was a vagal schwannoma before opening her up. Thus we (and she) willingly were prepared to remove the vagus nerve which is WAY more important to morbidity. Losing this would result in unilateral vocal cord paralysis and abnormal neural control of many abdominal organs. Thus, discovering that it was a sympathetic chain schwannoma was a great discovery for her. But, I like to keep things academic.
Weeks later during her follow up, she couldn’t be happier. The residents asked her about her new physical appearance and if it would lead to her having a hard time finding a husband. She laughed in their faces. The mass was more likely to take her out of the running, she thinks she looks beautiful. If a 16 year old girl can say that about herself, that’s the best surgical outcome possible. Enough said.
Like I had said before, prior to these events, I had never seen a sympathetic nerve schwannoma and even though their pathologies were exactly the same, the lessons learned from each were entirely unique.
In my second post in this blog over a year ago, I was reminded by a childhood friend to make sure I learn from every one of my patients. Looks like I listened to her.




I’ve been injecting schwannomas with lidocaine under ultrasound guidance and seeing what the temporary deficit is. I did one recently in a 16yo who had immediate unilateral VC palsy on flexible laryngoscopy and a hoarse voice. Lasted about an hour. She’s a singer so said she’d rather keep the mass for now than risk her voice. Also did a facial nerve and a v2 schwannoma, and injecting each had the expected deficits. I’ve never seen a sympathetic chain, but imagine it would work for that too.
LikeLike