Alright, I’m going to try to produce a series of “short” posts to get us all clinically caught up. I figured we’d start with the case I’ve hinted at many times; Amina and the hyena attack.
Two days before Halloween — although it’s not celebrated here it gives it an eerie context to me – I received a call from my residents that I needed to come in to evaluate a hyena attack. I had only seen a hyena once before in person, on my safari in Botswana ten years ago, but I knew they were all around Ethiopia. At night you can hear their somehow soothing but sinister calls to one another. The iconic hyena laughter we all know so well from the Lion King is a rarer sound. Anyways, it was around 10pm, so I found a bajaj and made my way in (this was when I still trusted bajaj drivers at night, before my attack).
She had already been placed into the OR and on the OR table by the time I arrived. When I walked into the dimly lit OR room I thought I was looking at a corpse. A still, cachectic human. The details of her entire skeleton were apparent. In my mind, I started listing bony anatomy as I was trained to do when presented with a skeleton. Diverting my attention as I walked towards the table, I examined for signs of life. There were plenty of them. Rapid, non-labored breathing, tachycardic pulse, and warm skin. Her abdomen and chest featured groups 4 parallel linear superficial, healing lacerations. They were clearly old, almost completely healed. Scanning up to her neck left me speechless….almost….“Fuck”
Here was an infected, saliva-enveloped, 10cm defect where her trachea and esophagus should be. Jagged pieces of necrotic cartilage reached out of the wound for help as they died. What was left of the posterior tracheal wall was lined with a white layer of infected debris. All of the tissue edges were pale white, clearly devoid of blood flow. Bubbling in the inferior portion of the wound made it clear why she wasn’t struggling. Her distal trachea communicated with the outside world and apart from fighting a salivary drip, breathing was easy for her. Looking up to her face, expecting to see sheer panic, instead, I was greeted with calm acceptance. This would start to make sense as my residents dictated her story.
This 55 year old female is from the Afar region. I knew a little bit about this area already. Literally, the first patient I saw when I arrived in July was an Afar gentleman with a massive myoepithelial carcinoma (his story is coming too). I spent a lot of time with Mohammed those first two months. The Afar have their own language apart from Tigrinya and Amharic that is completely different. Their region is mostly arid and their culture tends to be nomadic. Polygamy is practiced and for the most part, women do not obtain advanced education (or any for that matter). I visited this region while sight-seeing earlier that month; the sights and sounds were fresh in my mind.
The story continued. She was attacked by a hyena for unknown reasons 10 days ago. My mind now could connect the dots; the healing linear lacerations on her torso were claw marks made ten days ago and her tracheal defect had been bathed in saliva and exposed to the outside, dusty world for the past ten days. As they continued the story, I wondered how the hell she survived.
At the time of the attack, she presented to the local hospital (which by the way is only a 3-hour car ride from Ayder Hospital). There, she received first aid, basic IV resuscitation, and no blood products. Unable to take PO, say laid in that hospital for 10 days, slowly dying because “there was no transportation.” She arrived with a potassium of 2.5 and a hemoglobin of 4 (both well below normal and each alone is life threatening). The referral paperwork read, “Part of terachia taken by hayina”
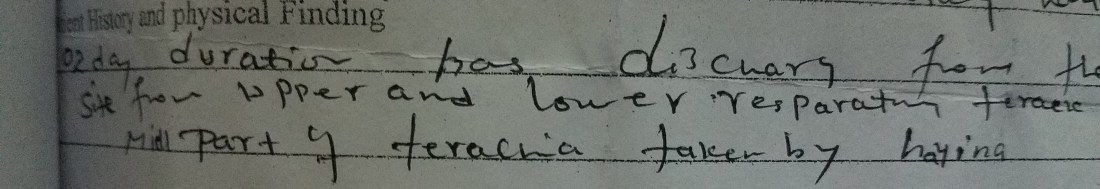
I could feel myself getting angry. I knew the line about no transportation was bullshit. Its impossible to think that something couldn’t be arranged for 10 days, there are great roads leading into the Afar region because of the tourist industry and Chinese-built roads. They expected her to die from her injuries and after she was still alive 10 days later, I guess they started to feel bad. Now, in our hands was a lady on death’s doorstep with the most extensive airway injury I had ever seen. By this time already I had seen plenty of people die here, but I was angry that I was forced to have her die at my hands tonight. Knowing I didn’t have to act that second, I stepped back to think for a second.
With her current condition, general anesthesia is dangerous so I thought to my time with time with trauma surgery during residency. “Get in, get out.” Do only what is necessary to keep them alive long enough to get the proper medical resuscitation. So, ABC. (Airway, Breathing, Circulation). Airway was easy, all we had to do was provide a stabilized access to the inferior part of her wound if positive ventilation would be needed. Simply cannulating with a trach tube would suffice since her trachea was wide open. Breathing wasn’t a problem either, her chest was mostly clear to auscultation apart from minor sounds of mucous bouncing around. Circulation, this was the problem. Severely anemic and clearly infected, she was most likely going to die from septic or hypovolemic shock at this point. The ICU team would help with the resuscitation, but antibiotics alone wouldn’t touch her copious necrotic tissue. This had to be removed in order to give her body a fighting chance against the infection. Then, the source of the infection (saliva) should be diverted away from the wound to prevent repetitive seeding of infection.
Thus, the plan was: 1. Secure the airway distally 2. Endoscopy to assess the extent of the injury and sources of salivary fistulae 3. Debride the infected tissue and find a way to divert the saliva away from the wound/airway.
As I explained the plan, I was told that there actually was a unit of blood in the hospital and that it was on the way. Wonderful. I smiled as the anesthesia team positioned themselves at the head of the bed with the laryngoscope and endotracheal tube in hand. It was a much needed comic relief for the tension I was feeling. As she fell asleep, I took the breathing tube from them and gently slid it through the wound into the distal trachea. “Easiest intubation ever,” I declared. They weren’t amused.
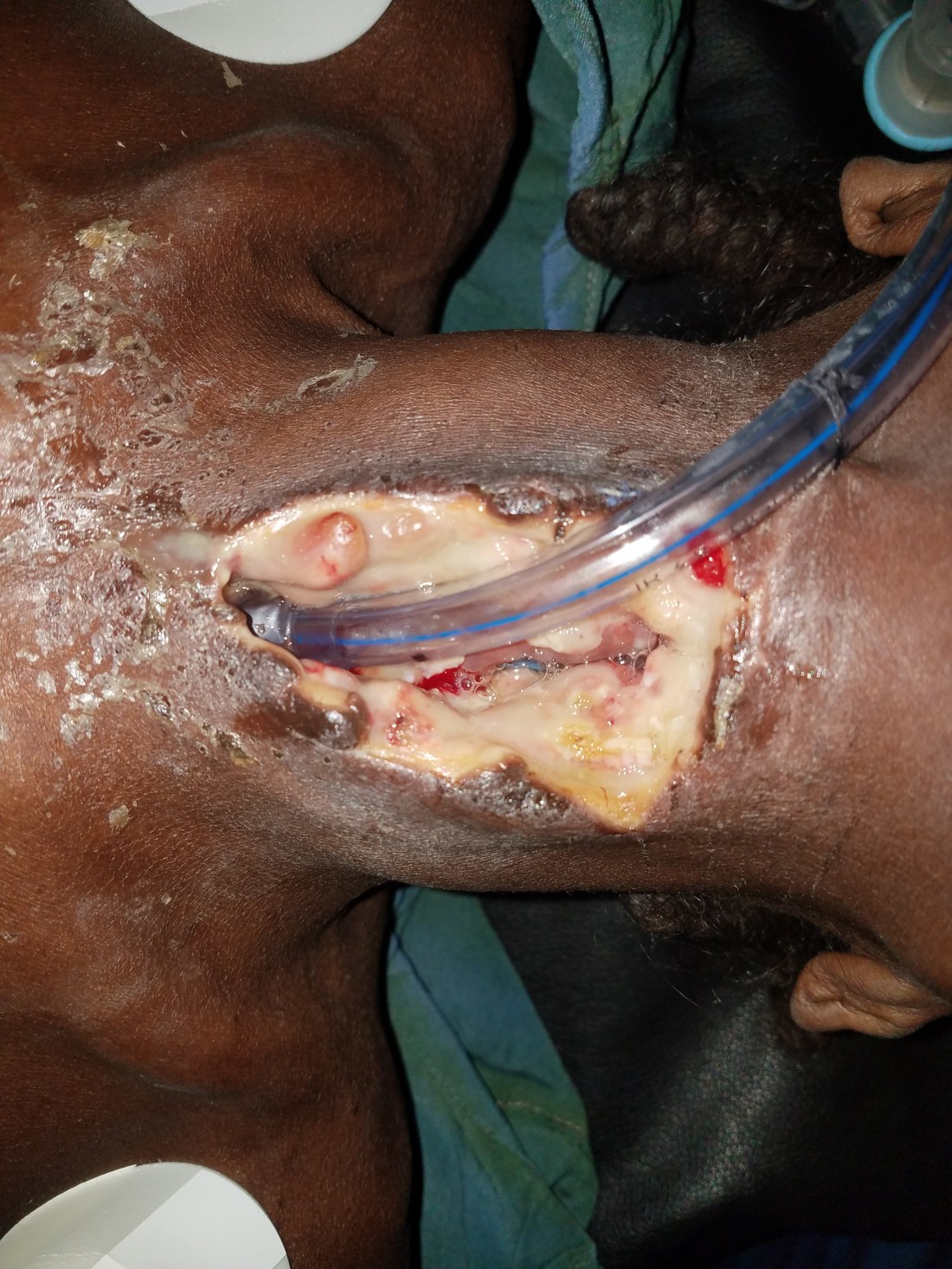
The anatomy is outlined in this video, but simply distilled, the hyena had removed her entire larynx and the anterior two thirds of 5-6 tracheal rings. The distal opening into her airway was just beneath her sternum. All that was left of the supraglottis were here arytenoids and epiglottis. The anterior esophageal wall along the same length had been ripped open. Almost like a single tooth unzipped the anterior wall. The distal airway was normal to the carina. After endoscopically cannulating the esophagus with a large nasogastric tube and confirming its placement in the stomach with insufflation, we documented again. You can see the blue-clear plastic of the NG tube peaking through the esophagus.
Next, we quickly and aggressively debrided necrotic tissue until we found healthy, bleeding tissue. The two sources of saliva were clear now. Through the supraglottis/piriform sinus and the anterior esophageal wall. Quick running, locking suturing of both areas. Placement of a big 10 DCT trach distally. And we used tracheal cartilage and skin to close off access to the distal trachea and left the superior part of the wound open. Thus, the path of least resistance for saliva would be through that superior open wound and away from the airway. It wasn’t pretty.
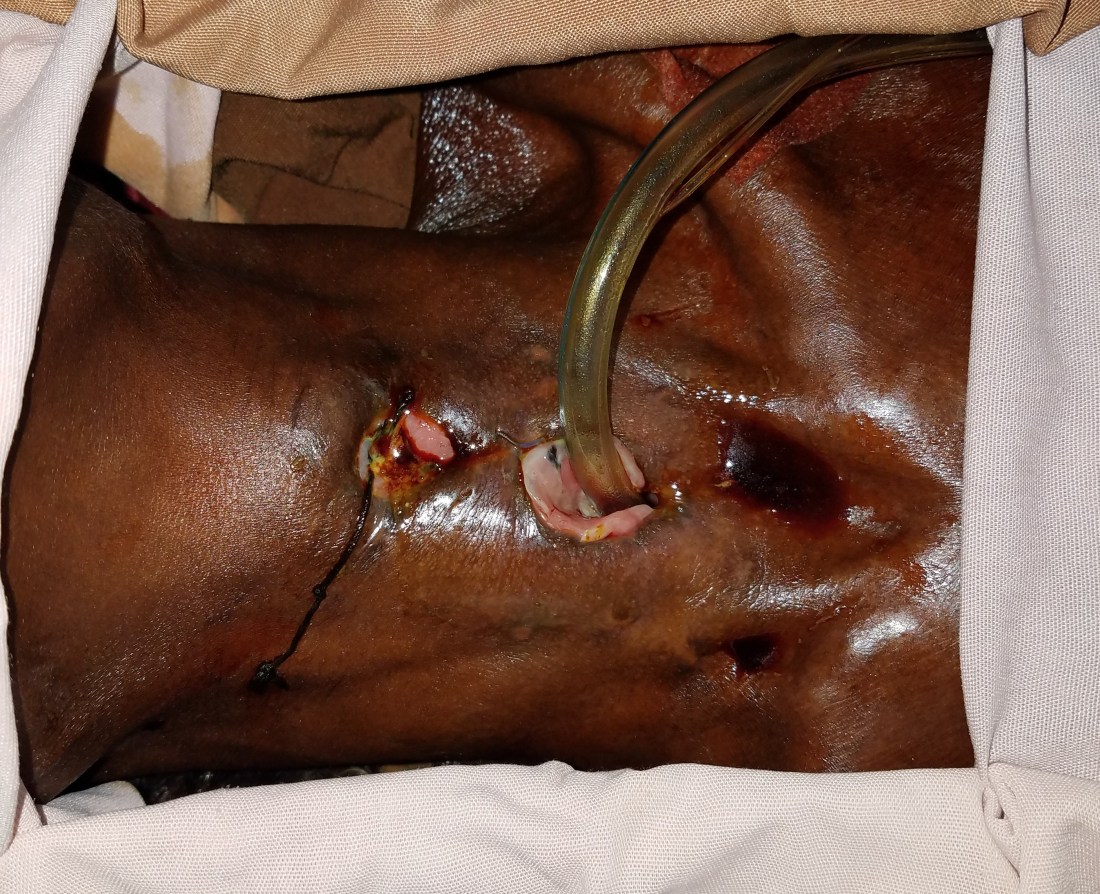
I called my dad after it was done to get his advice on antibiotic coverage (it was still the evening in the US). As an infectious disease specialist for over 35 years, he has an amazing library of knowledge and intuition that I love to query. My international consults to him have been challenging, I think, and this was another first for him. Antibiotic coverage for hyena bacteria? The call was less for medical advice and more for moral support. It did the trick.
The next couple of days was very rough for her. Battling sepsis and severe electrolyte imbalances, she struggled through delirium and coping with the reality that she might live. As she improved, it became clear to me that she didn’t want to. Every time I’d reach out to treat her, she would fight me away, signaling me with hand movements to pull out her trach tube and let her die. Unfortunately, at this point, it wouldn’t be that easy to die. She’d somehow gotten past certain death and was recovering. Seeing her clear distaste for being alive, I contemplated my rationale for keeping her that way.
As the weeks passed and the salivary fistula lessoned, infection disappeared and her energy increased; it was now clear that she will survive this event. Feeding her was an issue since we could only use the nasogastric tube. We consulted our nutritionist who did everything she could to get calories in liquid form, but eventually, the diet consisted of multivitamins, whole milk, and water. It seemed like she physically couldn’t gain weight. I explained to her that what we did in the first surgery was just a patch and if she ever wanted to eat or return home safely, we’d need to separate her airway from her digestive system. Here began the biggest problem. She understood a dialect that very few others could and should couldn’t speak or write. She needed to ask questions with hand gestures. It wasn’t easy.
Finally, with all questions answered we moved into a second stage procedure. After a lot of international consultation, the consensus was to remove the remaining injured tracheal cartilage and mucosa (because its still producing mucous and would create a mucocele under any reconstruction perhaps), to separate the distal airway from the proximal airway and create a new opening in the skin (mature the tracheal stoma). We do this often for laryngectomy patients, but never had I done it for trauma. At the same time, we’d repair any leftover fistulae and esophageal injuries and formally close off the hypopharynx from the rest of neck. From now on, the mouth would only connect to the esophagus. Ideally, we’d throw up some extra tissue like a Pec flap or a supraclavicular flap, but these were physically impossible in her cachectic state.
As you can see from the pictures, the skin wasn’t healthy, there was a persistent fistula through the glottis and anterior esophagus. We did our best to repair the holes and provide the airway a safe place to live. I had no idea what to expect from her recovery.
3 weeks after her repair, I reluctantly removed the NG tube and performed a barium swallow. No leaks…
The next day she was shoveling injera with shiro like nothing ever happened. Her attitude completely changed. She’d strut the hallway all day with a childish grin. Not only did she cheat death, but she was the lady of the hospital. People from her region would visit, she’d interact with all the other ENT patients and overall just seemed happy with life. I used to be greeted with a look of fear (or distaste) on rounds, but now each time I turned the corner, I’d receive the same huge smile filled with carefully sharpened teeth (people in the Afar region shape and sharpen their teeth).
We had a cleft palate/plastics mission visit while she was here and I could tell how proud she was when we presented her on rounds to the huge group. She was given a brand new soft laryngectomy tube by the visiting team and that’s when I realized that she didn’t need us anymore.
She had survived a hyena ripping out her larynx, 10 days without real care and 2 completely experimental surgeries. I can’t explain how she survived. Surgeons aren’t supposed to admit when they don’t know what they’re doing but this was certainly the truth. Every time I think back on her whole case I always say to myself, “shit, that was crazy.”
Now that she’s back in Afar at home, I often daydream about how she’s coping with her new life. I’m pretty sure she won’t return to Ayder hospital, but I really hope she decides to visit. I’ll never forget my 3 months with her nor will I ever be able to explain just how much shes taught me about life.


