This post I will keep brief since most of the clinical happenings this week consist of incomplete stories. So, I’ll give a couple updates on patients and present my next extremely challenging pediatric case.
Let me begin with a bit of venting. The first emergency case I did here in my 2nd week was a pediatric trach for bilateral vocal cord paresis secondary to a Chairi II malformation.

Now, over the last month, our team has made a tremendous effort in teaching trach care, doing trach changes and rounding on this child daily. About two weeks ago I noticed that she was visibly losing weight. The ICU is run by a constantly rotating staff of interns, so maintaining good patient care or even consistent communication is very difficult. Every day, I had our residents communicate the necessity of weight gain, good nutrition, and daily weights. This rarely happened and I could never get a straight answer to why. What’s frustrating is that I’m no expert in neonatal care and nutrition, but I knew whatever they were doing was not enough and they needed to do better. I thought my constant rounding, face to face talks and conversations with the attendings would manipulate behavior. It didn’t.
Last week, the PICU intern reveals that they have been fighting persistent fevers without a source for 10 days. This was news to me because the temperatures recorded on the bedside vitals sheet were normal. My first instinct was to check all the surgical sites. The trach I knew well and the stoma was still very clean without ulceration. The occipital decompression site was clean and dry (although the sutures were still there from 3 weeks ago). A check of the lumbar incision for the removal of the myelomeningocele reveals partial dehiscence and fullness which leaks clear fluid on palpation. THERE’S A CSF LEAK. This surgery was 3 weeks ago. There have been fevers for 10 days and the attending Head and Neck Surgeon is the one to find the NSGY complication and likely source of fever. I was furious.
I pulled everyone in the PICU over to see. None of the nurses or residents or interns had appreciated it before and none seemed shocked or worried by its presence. I had my residents call NSGY to inform them of the complication and to move them to action. Six days passed without a clear plan or intervention despite daily inquiries from our team. It was clear to me this child was dying and there was nothing I could personally do about it. Over the past month, I have watched this child slowly die in front of my eyes. Friday night, she went into cardiac arrest and passed.
For our department’s first ever Morbidity and Mortality conference this month, I will feature this case. This child and the sight of her cachectic body will haunt me. Yes, it may have been difficult to get her decannulated and there was no telling what her neuro status would be, but she shouldn’t have died like this. Failure to thrive from malnutrition and iatrogenic CSF infection are not only preventable but very treatable. I’m upset and not quite sure what to do with it yet.
Why don’t we change the tone and move onto other topics…
My Illness:
It’s gone! I finally have energy again, can breathe through my nose and don’t have to constantly take medications to do my job. The Ethiopian Gunfan….not to be messed with.
The child with GBS:
The 4 year old I mentioned in last week’s post was able to wean off the vent in just a couple of days. Unfortunately, he developed decreased aeration of the right middle and lower lobe and needed to go back on the vent. Since he was stuck on the vent and the portable xray machine had been down for a while, our team was called to bedside to help. In the states, I’d turn to the PICU and say “you can handle this better than me”, which is true! But here, it’s different. Ventilating a trached pediatric patient is a brand new concept for the pediatric interns and residents looking to me to help. The uncuffed shiley that we placed for lack of another option wasn’t helping. Without the cuff, the amount of positive pressure and PEEP that was needed to recruit alveoli was limited by air escaping from the mouth and nose. While I asked the team to find a 4.5 cuffed ETT, our residents rummaged around the airway supplies stored in a random bag in the back of the room. There, they discovered a 4.5 cuffed flextend bivona.
Amazed with this treasure, I popped a syringe and asked the mom for her water bottle (The bivona balloons require sterile water rather than saline…we don’t have sterile water). Filled the syringe and tested the balloon. I had no idea how old this trach was, but it worked. Used a free 10 blade to pop open the trach ties (it’s impossible to find scissors) and completed the trach change. The tidal volumes increased and we gave a couple bigger requiting breaths popping open the right lung. Very simple fix to a relatively complex problem. Remember, he already had subglottic ulceriztion from the ETT, so I didn’t want to leave the cuff up for long. I’d let him ride for a couple of days with the cuff and try then to lower it again.
Our friend with the neck ulcer of unknown etiology goes home for the holiday!:
As the only patient to be featured in all my medical posts, I have gotten to know this gentleman pretty well after a month. As you review the pictures, you can see that we went from an ulcerating mass from hell to a life-threatening necrotizing bacteria.
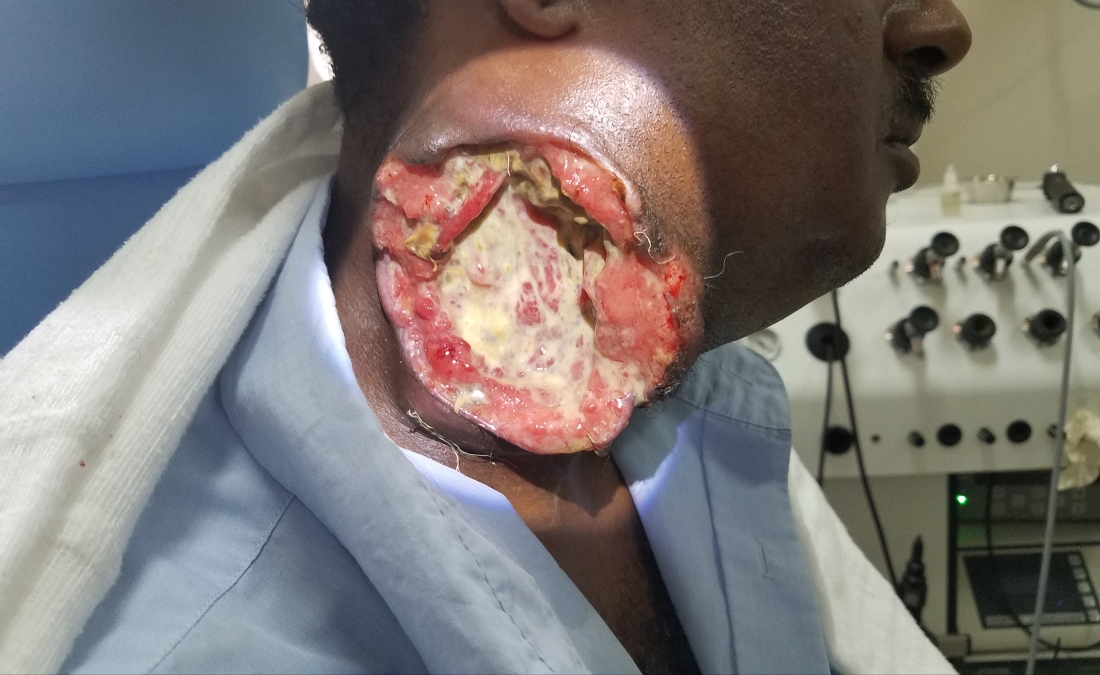
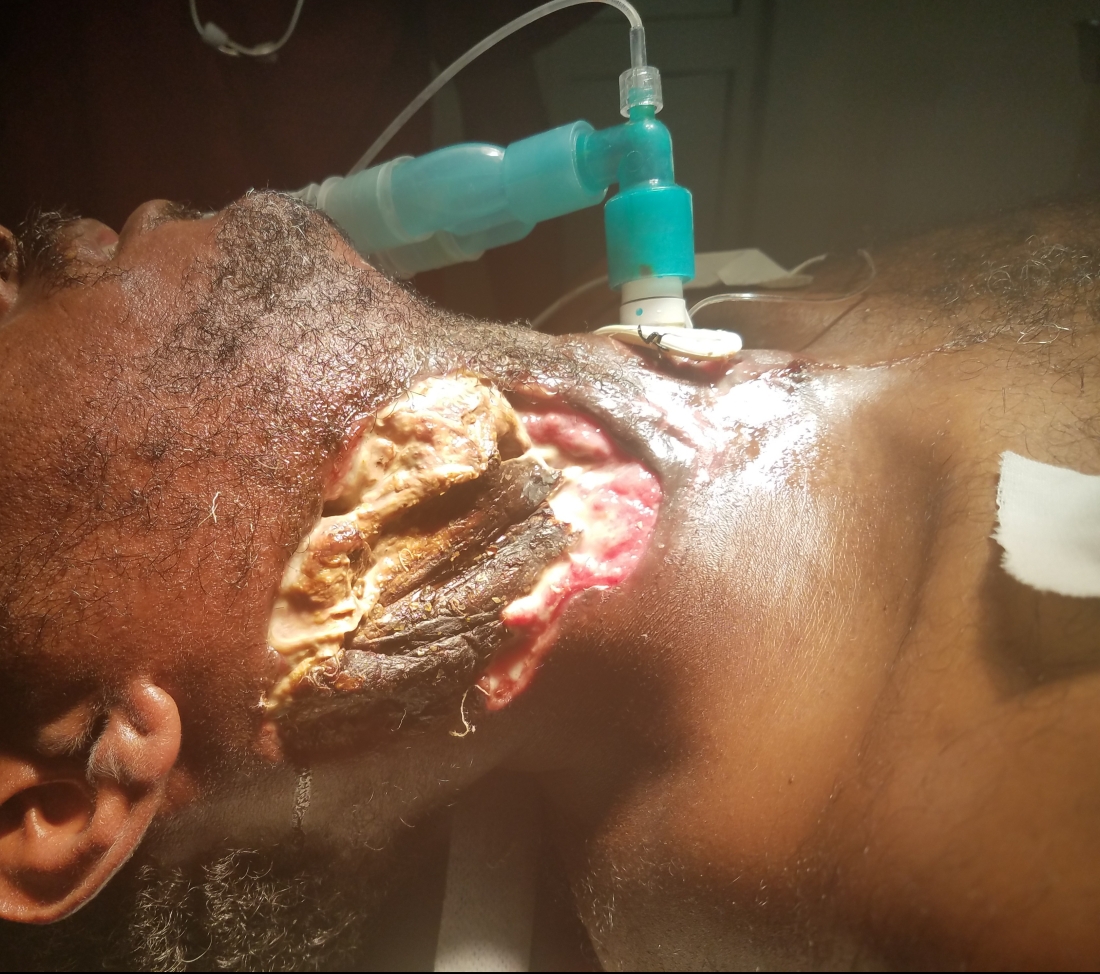

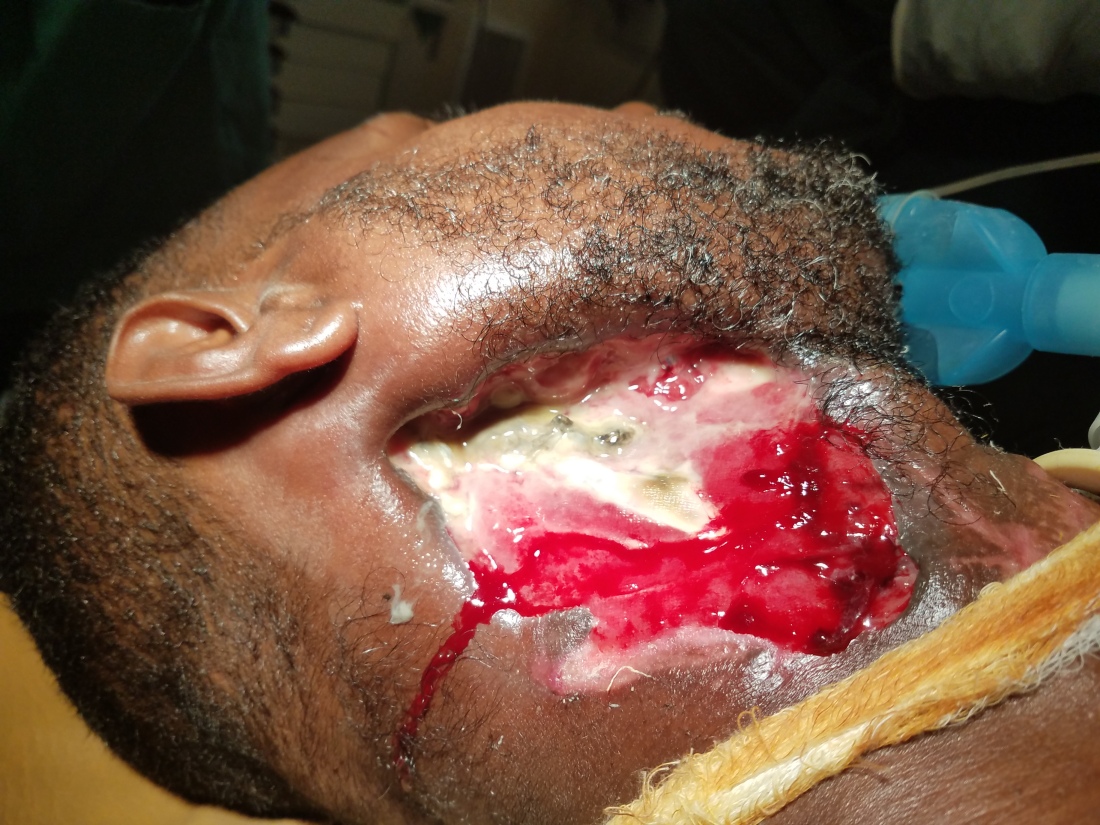
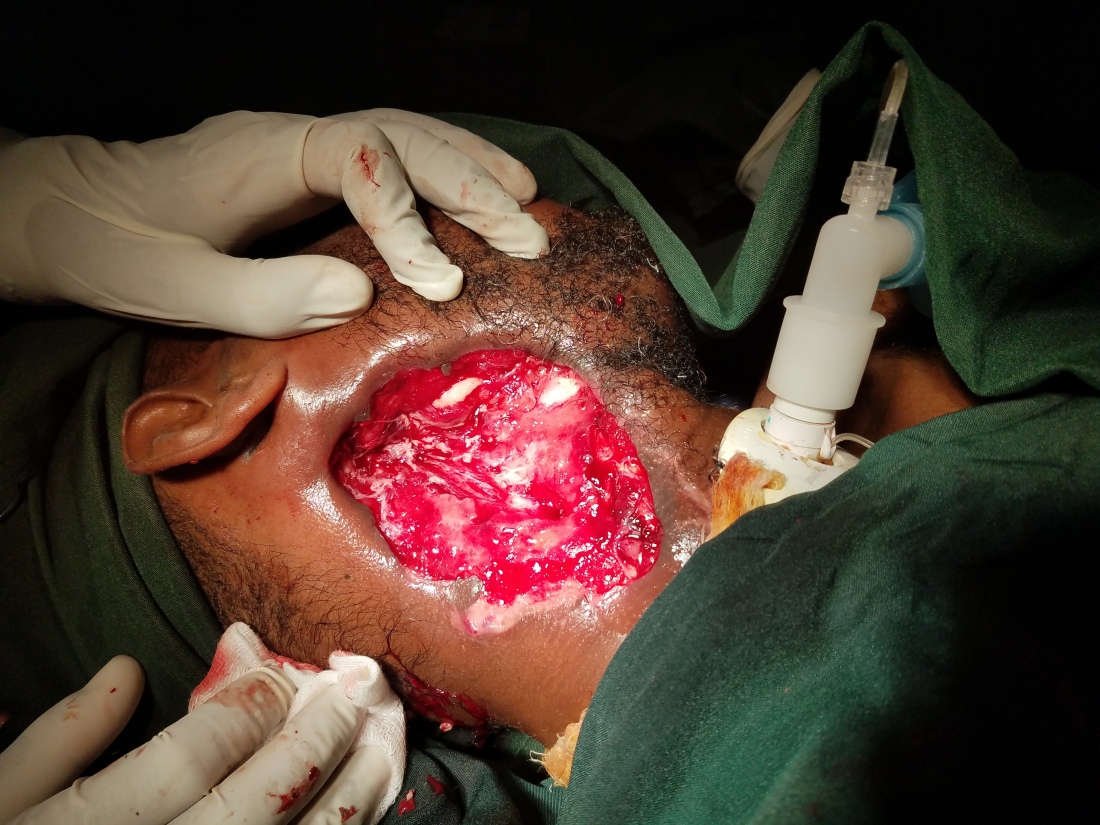

After our first debridement, I was so concerned for an imminent carotid blowout that I contemplated a prophylactic carotid artery sacrifice and had a long conversation with him about life after a major stroke. Luckily, it never happened and during the subsequent debridement, the carotid was protected by granulation tissue. Now, after weeks of excellent wound care by our team, the Ethiopian new year was approaching. I asked him if he had any desire to go home for the holiday (he lives quite far away) and if there was anyone to take care of him at home. That’s when he dropped the biggest bomb of his month here with us.
He politely said, in Tigrinya as translated by my residents “No, everyone is busy at home. My wife just gave birth 2 weeks ago.” My face must have somehow expressed both shock and pure joy at the same time. This man, who somehow avoided one of the most dramatic ways to die by a microscopic layer of inflammatory granulation tissue has a new baby at home that he has never even seen! I had to step out of the room for a second to control my lacrimal glands (this has been happening a bunch here…). I step back in, staring at him, determined to find a way to get him home. I take out his inner cannula and occlude his trach. Since the inner canula was sitting in a fenestrated trach, the superior fenestration now allowed air to freely move past his trach and larynx with ease. Had him say hello and then goodbye to his trach. He was excited about the decannulation. Over the next two days, our team taught him and his bedside family how to do the daily dressing changes. On Friday, he thanked us and promised to return in a week. My only demands were that he kept taking his antibiotics and to bring me back baby pictures.
The airway foreign body selfie!
A couple of weeks ago I posted about the pediatric general surgeon asking me to assist with a chronic foreign body. During that case, there was this excellent picture of one of the general surgery residents taking a moment to take a selfie during a key moment of the case. Well, the senior general surgeon asked me to join him again for a fresh pediatric foreign body and I found that resident and got his perspective. Its almost like the famous Matrix rotational camera cinematography trick…but not really.
Also in that post, I was very concerned that I burned a bridge with this general surgeon because I took over that case. Well, this time around, I changed my teaching technique and he was able to perform a very smooth extraction of a piece of jagged metal from the right mainstem bronchus. You could feel the pride in his confidence and his request to share Buna with me afterward solidified our friendship. These cases generate a lot of excitement, so during a stable segment of the case, I stepped back to snap a picture of everyone else taking part in the case.
2 New Cases:
The fun one:
A 1.5 year old with a large off-center mobile, slowly enlarging neck mass. They don’t save the US video here, but the report suggests that a cystic structure was deep to the SCM, deviating the trachea to the contralateral side and obscuring the ipsilateral superior thyroid pole. It sounded like a branchial cleft cyst and possibly a type III. If I had an ultrasound myself I’d confirm it, but surgical excision was indicated for its size, mass effect and recurrent infections. Although I was also mentally prepared for a thyroglossal duct cyst procedure, it indeed turned out to be a 3rd branchial.
To review, there are 4 types of branchial cleft cysts that are categorized by the embryologic brachial structures they grow between. The 1st branchial cysts involve the ear canal and the parotid. The second travels from the crypts of the tonsil, between the internal and external carotid artery and follow down the SCM superficially. The 3rd and 4th types both exit the piriform sinus and run deep to the SCM along the carotid sheath. Once they reach the thyroid, any number of things can happen, but in this case, it just barely involved the superior pole of the thyroid.
The excision requires isolating the tract leading to the piriform and careful ligation to avoid re-accumulation or a fistula between the hypopharynx and neck. It was a fun procedure and reminded me how much I love pediatric soft tissue cases.
The scary one:
A 3 year old was brought to our OPD from the ER Wednesday afternoon just as it was closing. I had already left to catch my bus, but when I saw a text from Seid I knew something wasn’t good. It read “Doctor, could you please come back to the OPD.” I arrive to see the near lifeless 3 year old in the arms of her extremely worried mother. Beneath the flies seeking necrotic tissue, I noticed a black hold just under the left medial canthus. After I angrily swiped away the flies, I appreciate generalized skin abrasions, dried blood from the left naris and an angry oozing ulcer of the left lip. She was dehydrated, malnourished and septic. The hole under her eye reached into a deep sulcus. Palpation returned copious purulence and the presence of eroded bone. The haze of purple forming around her lower lid was a demarcation of necrosis. The only other finding featured a similar, smaller necrotic hole in her left soft palate. Although this seemed insignificant in comparison.
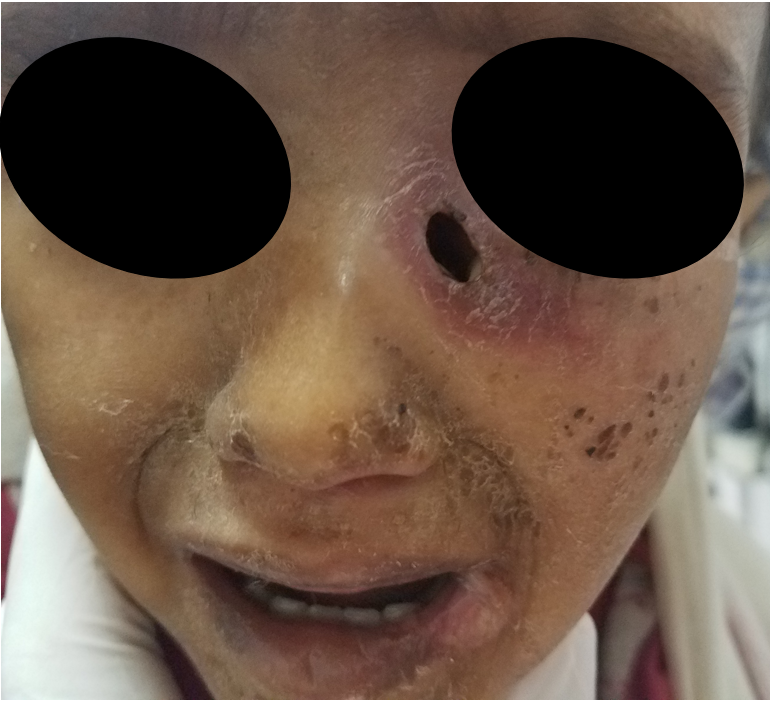
My best guess was this was a dacryocystitis superinfected with an aggressive bacteria in the setting of an immunocompromised state (be it from malnourishment or HIV, or both). I admitted her to the pediatric ward, started broad spectrum antibiotics, screened for HIV (negative), placed an NG (right naris), obtained a CBC (slightly anemic with a WBC of 20 with a strong neutrophil shift) and other basic labs and had them set her up for the OR the next day…first case. She obtained a CT overnight that showed a fistula formation from left nasal cavity to just under the eye. Right where the lacrimal duct runs.
Well, of course when I show up in the morning, the peds team had just fed her a bolus of formula so we had to wait for 6 hours (these little clinical mistakes are unbelievably frustrating).
Anyways, once we finally got to the OR, debriding the necrotic tissue revealed a partially eroded orbital rim and exposed, but intact orbital septum. There was dehiscence into the anterior ethmoid and the medial wall of the orbit was partially exposed and dehiscent. An endoscopic look into the left verified our suspicions. There was clear tract of partially necrotic tissue emanating from the undersurface of the inferior turbinate. Lifting it dorsally revealed copious purulence and a trail of destruction from the lacrimal duct to the inner surface of the turbinate to the nasal floor. All of this was debrided and an inferior medial maxillectomy was performed to open the maxillary sinus.

The difficulty, I have now learned after many infectious cases, is that you have to rely on your clinical judgment in selecting the likely infectious organism. For the reliability of even the gram stain here is extremely low. Not to mention that I’m told there are no fungal cultures and KOH stains are only done in the dermatology clinic. Pathology doesn’t do AFB, silver stains or really help at all in an infectious workup. Seems like this should be a strong focal point for the hospital. Infections are very common here and their evaluation/workup should be reliable. I made a mental note to look into this in a little more depth.
Although I was pretty sure this was bacterial in nature, fungal and AFB infections were still very high on my differential. As I often do, I called my father for his intuition. He’s been a pediatric infectious disease specialist for a very long time and his initial intuition always seems right. My fear revolved around something I noticed when I was down in Addis. During our trip, we visited the St. Paul Head and Neck team which shared a building with dermatology. Well, the dermatology clinic has a poster on the window discussing noma with large disturbing pictures of the devastation of noma. Simply put, noma (meaning “to devour”) describes a type of necrotizing ulcerative stomatitis. Kinda like gangrene originating from the oral gingiva. The end results are devastating and require significant facial reconstruction. Malnourished children are especially susceptible. But, even though our girl had infectious oral findings, the epicenter still seemed to be the lacrimal system and was probably unrelated to noma. Nevertheless, I was on alert and knew this girl was critical and still nowhere near out of the woods.
The wound was packed with xeroform and dressed. If she’s able to battle past this infection without it spreading to the eye, then the real discussion begins. How do we reconstruct? Is there anything I can do to repair the lacrimal duct during the repair? This will be a discussion for next week. If anyone has some good ideas, please let me know.
And….puppies









My hat’s off to you sir! I am impressed with your altruism and dedication! (I am an ENT in FL… leading a comparatively cushy life).
LikeLike